Note to readers:
Zainab Edwards is an ice skater.


It runs in the family. Edwards’ mother, Cynthia Elliott, grew up on the ice in Minnesota and her older daughter skated competitively for years. So when Elliott and her husband Dave agreed to foster Edwards five days after her fourth birthday, the little girl was in skates almost immediately.
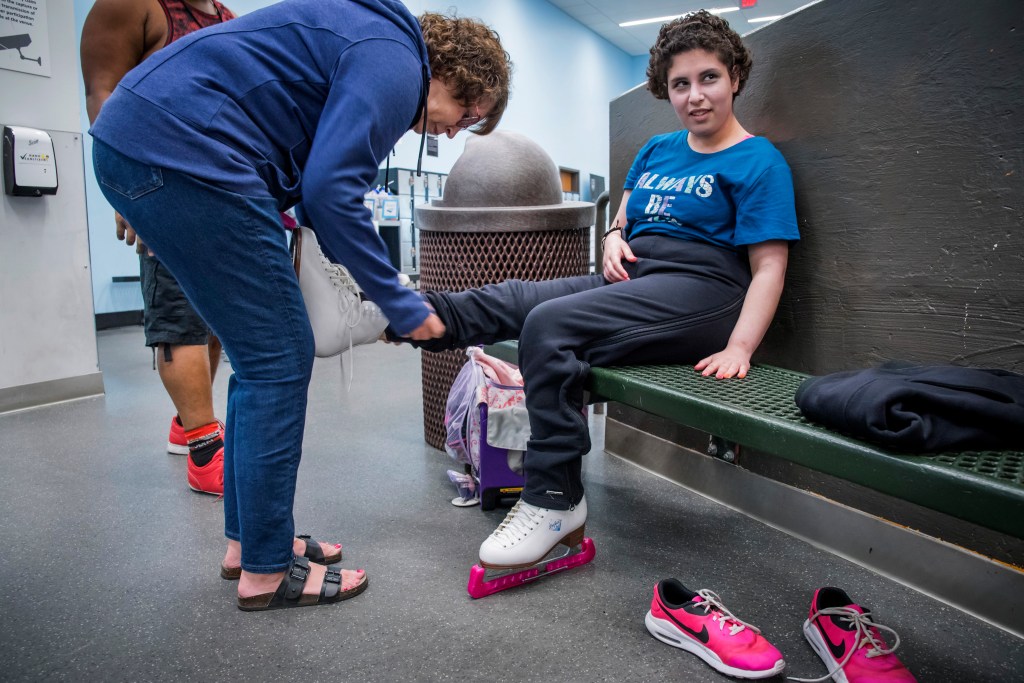
On a hot spring day in 2021, Edwards, 23, stepped gingerly onto the ice at a rink in Chandler, Arizona. The place was nearly deserted – perhaps due to COVID-19, or maybe because it was a Thursday morning. Pop music blared from the speakers as Edwards moved slowly, led by an instructor who faced her, holding both of her hands.
Edwards smiled. Elliott exhaled.



This was a good day, though the young skater did wave away a request to talk with a reporter.
Edwards has had challenges her entire life. She was born profoundly deaf. Digestive issues led to the removal of her colon; she has an ileostomy bag for life.
For many years, American Sign Language and, later, cochlear implants, allowed her to engage with the world. She flourished – visiting Disneyland with her family, making friends at school and participating in Special Olympics.
In 2014, everything changed. Edwards began to have difficulty walking and picking up objects. She could no longer tolerate her cochlear implants. She began to have hundreds of uncontrollable seizures each day. She became combative, lashing out physically at caregivers and her mother. At one point, her condition was so bad she couldn’t feed herself.
It took years to figure out what was going on and by then, it was too late for a full recovery.
In 2017, Edwards was diagnosed with autoimmune encephalitis, a rare, hard-to-detect condition sometimes called “brain on fire.” Caught early, the effects can be reversed. For Edwards, it was largely too late.
Physical therapy allowed Edwards to ice skate again, and ride her bike.
“She still can’t write her name,” Elliott said. “She’s lost all those cognitive skills. Those have never come back.”
Unable to keep her daughter safe at home and concerned about what will happen when she and her husband are no longer around to care for her, Elliott, now 71, began to look for a permanent living situation. After a lot of research, she and her husband purchased a townhouse – close to their home, walking distance to a park. The plan was to have the young woman live with a roommate – both for company and to offset costs – with caregivers and other services provided by the state of Arizona.
That never happened, dashed by Edwards’ aggressive behavior.
Depending on an individual’s needs, some families are able to pay out of pocket for services. But in many circumstances, that’s impossible – leaving family members to care for a loved one round the clock.
About 7.4 million people with intellectual and developmental disabilities live in the U.S. Of those, only about 1 in 5 receives paid supports from a state agency, according to a 2017 U.S. Department of Health and Human Services report.
Most Americans with intellectual and developmental disabilities get nothing at all. Others languish for years on waiting lists.
But Arizona’s unique structure of services means that the state pays more than a million dollars a year for Edwards’ care.
And yet Edwards’ family says her quality of life is dismal. Even when funding is available, there are vast disagreements in the disability community about what constitutes an appropriate living setting, let alone specifics regarding care.
How to create a healthy, happy community setting for an individual with complex behavioral and medical needs is a political, philosophical and economic conversation that often goes unheard.
As of September, Edwards had two round-the-clock caregivers and a third during the day, all three fluent in ASL. She also had a nurse and sign language interpreter for the nurse, both 24/7. A behavior coach was with her 40 hours a week, along with another translator. This – along with medical costs and transportation — is almost all paid for by the government.
When spending that amount of money on services for one individual still can’t provide a safe, happy and productive life, it calls into question how the money is being spent and the assumptions underlying state policies on care.
Because of high staff turnover and insufficient training, Elliott said, she still provides almost constant care for Edwards — administering medication, grocery shopping, planning outings, making doctor appointments and dealing with trips to the emergency room when Edwards’ behavior spins out of control.
At least 60 different staff people have been in and out of Edwards’ home in the last couple of years, Elliott said.
Between January 2018 and January 2022, the police were called to Edwards’ house more than 100 times.
“The behavior following some of her seizures is extreme, she has kicked out the van windows, broken her bedroom window that was plexiglass, she will hit, kick, bite, pull hair,” Elliott wrote in an email to the Center for Public Integrity.
Even when there’s no health crisis, Edwards’ quality of life isn’t great, her mother said.
The young woman is surrounded by caregivers, but according to Elliott, it’s rare that anyone attempts to engage with her daughter. Elliott says she has to push staff to have Edwards help with household tasks like emptying the dishwasher or folding clothes.
After Edwards got second degree burns on her hands and her mother was unable to determine what happened, Elliott installed five cameras in Edwards’ home. She said there hasn’t been a similar episode since – but the cameras show how isolated her daughter is.
“It’s heartbreaking to see Zainab sitting alone at the kitchen table eating a meal while three staff sit in the other room on their phones.”
The hardest part, Elliott said, watching Edwards move across the ice, is knowing her daughter is capable of so much more.

Searching for solutions
Generations ago, Zainab Edwards would have been sent to live at the Arizona Training Program, the state’s institution for people with intellectual and developmental disabilities, which is a one-hour drive from Phoenix, or maybe to the state mental hospital near downtown.
Edwards would have been isolated from her community, either by distance or razor wire. Forays off an institution’s grounds would have been rare and poor behavior would likely have resulted in physical restraint and isolation.
Instead, as a result of decades of reforms and a landmark 1999 U.S. Supreme Court case, federal regulations call for states to create mechanisms that help people with disabilities live among members of their community.
In that case, Olmstead v. L.C., the court said that under the Americans with Disabilities Act, segregating people with disabilities who could live in the community with supports was discrimination.
Technically, Zainab lives in her community. But in many ways, she’s in an institution of one.
The reality is that people with the most complex needs and, particularly, aggressive behaviors, are often isolated from the rest of the world, even when their living situation technically fits within the letter of the law.
Although services are funded through Medicaid, each state has its own method of delivery. Arizona, where Edwards lives, is considered one of the best because it allows anyone who qualifies for services to receive them immediately. Unlike most other states, Arizona has no waiting lists.
In 2018, the state created an “Enhanced Transitional Group Home” model, designed to devote extra resources to support people with complex needs.
But that does not necessarily mean that Arizonans with intellectual and developmental disabilities are getting what they need.
The Center for Public Integrity obtained a copy of a 2019 study of individuals in Arizona enhanced group homes. In a review of eight people (not including Edwards, though she’s in a similar setup), a researcher concluded that seven of the eight were no better than they’d been in previous settings:
Related story
Court victories deliver cautious hope for voters with disabilities
“The members did not make significant behavioral gains in either reduction of challenging behaviors or acquisition of social and self-determined competencies” and that “staff and member engagement in participatory, meaningful, and functional activities was staggeringly low.”
A young woman referred to as “RS” was one of the eight people studied. She has autism and mental illness, and often has aggressive behavior.
The researcher said RS’s caregivers were engaged with the young woman only about 30% of the time – slightly higher than the average of 25% among the eight people studied.
“During the observations, RS predominantly sat by herself looking at her iPad,” the researcher wrote, adding that the young woman had continued to harm herself and others, despite a high staff ratio.
The group home “has not improved [RS’s] quality of life in over 14 months,” the researcher concluded.
An accounting by the state obtained by the Center for Public Integrity showed that at more than $87,000 a month, RS’s care, like Zainab Edwards’, exceeded a million dollars a year.
Despite the large amounts of money being spent on services for people state employees have internally referred to as “Complex Carls,” caregiver pay remains low.
Critics say oversight is lacking and regulation inadequate.
“It is clear to anybody with eyes that the way things are being handled right now simply isn’t effective,” said Jon Meyers, executive director of the Arizona Developmental Disabilities Planning Council, which advises the state on issues facing people with intellectual and developmental disabilities.
Meyers said that high turnover among caregivers, which he blamed on low pay and a lack of training, is one of the most significant challenges facing the system. Simply adding staff members, as has happened with Edwards, isn’t enough, he said.
“It is not just a matter of not having enough money. It’s a matter of using the money wisely,” he said. “We are often just throwing money at it without knowing what is going to be effective.”
There’s another element, too, Meyers said – “questions we don’t yet have answers to. There are people whose diagnoses are so complex that right now we can’t fully provide for them. We can’t fully provide the care they need.”
A spokesman for the state didn’t address questions about the million-dollar price tag for services for some people with intellectual and developmental disabilities, but did acknowledge that the initial project was not perfect.
“It is not just a matter of not having enough money. It’s a matter of using the money wisely.”
Jon Meyers, executive director of the Arizona Developmental Disabilities Planning Council
“While there were aspects of the pilot model that were more successful in providing individuals with an engaging living environment where their needs were supported, the Division continued its work to improve and enhance this service model,” said Brett Bezio, deputy press secretary for the Arizona Department of Economic Security, which oversees the Division of Developmental Disabilities. “Using the information and trends that were identified in those initial years, review of models in other states, as well as working with external experts in this field, the Division has created an updated service specification for this type of residential placement setting that it hopes will make the service more effective in the future.”
Finding, training and adequately paying caregivers is a nationwide challenge.
A workforce shortage of unprecedented proportions has challenged just about every state to provide care for its most vulnerable residents. Just before the pandemic, a survey by ANCOR, a national trade association that represents care providers, showed that almost 70% of caregiving agencies could not provide the services needed. The problem only worsened during the pandemic.
Because of low pay and staff shortages, a disturbing trend has emerged, said Barbara Merrill, chief executive officer of ANCOR.
“[States are] closing the smaller three-, four-bed group homes and moving people into [larger] group homes,” Merrill said. “And that is going in the wrong, wrong, wrong direction. It’s not what we’re trying to do as an industry, it’s not what we’re trying to do as a country.”
At the same time, institutions across the country are closing. In Washington state, families and guardians are concerned that as congregate care facilities shut down, there are few alternative placements.
A 2012 University of Minnesota study outlined the challenges for families of people with complex behaviors. The conclusion could have been written today.
Families “often have difficulty in keeping jobs; can have limited opportunities for socialization, friends and family due to social isolation; may be sleep deprived because their children are up all night; and may encounter frequent injury such as bites, bruises, hair pulled out of their heads and even broken bones,” researchers wrote. ”Even in these crisis situations, families wait for services.”
In other words, easier said than done.
Amy Hewitt, who worked on the study, is the director of the Institute on Community Integration at the University of Minnesota. She recalled a situation involving a man with developmental disabilities who had several staff members – and a similar outcome to Zainab Edwards.
The man’s caregivers were so poorly trained and ill equipped, Hewitt said, they were afraid of him.
“The staff would run and hide in the bathroom, in the kitchen, in the staff area. There’d be five of them.”
And the man was not integrated into the community.
“He had an exercise program where he would just walk the perimeter of the inside of his bedroom over and over and over and over,” Hewitt said.
“You can throw all kinds of money at something, and it’s not going to make it work if you’re just doing more of the same, which is sort of glorified babysitting,” she added.
“From that kind of money, you could buy the best behavioral consulting the world had to offer.”
Good intentions simply may not be enough.
“Having philosophical values is fine,” said Bob Kafka, a longtime organizer with ADAPT, a grassroots disability advocacy organization, “but where the rubber meets the road is how you’re going to implement it.”
Mobilizing against mistreatment
Society has never known what to do with someone like Zainab Edwards.
Historically, people with disabilities were isolated, mocked and abused.
The emphasis on science during The Renaissance led to a greater understanding of disability, and later philosophers studied people with cognitive challenges as a precursor to the development of the field of psychology.
That didn’t necessarily translate into better living conditions.
Dorothea Dix, a social reformer in Massachusetts in the mid-19th century, was horrified by living conditions for people with mental illness and intellectual and developmental disabilities. Her work led to the creation of public institutions for them and people with mental illness – to the chagrin of later generations of advocates.
Arizona’s State Asylum for the Insane opened in 1887. In 1912, the year of statehood, the asylum’s annual report listed 375 residents and included obvious cases of intellectual and developmental disabilities.
In the late 1940s, right around the time that Arizona’s leaders were considering building a separate institution for people with such conditions, controversy arose. Conscientious objectors to the draft in World War II were instead assigned to work in institutions, and spoke out about poor conditions. In 1950, families came together to form the National Association for Retarded Citizens, now known as The Arc of the United States, and began mobilizing against mistreatment.
The disability rights movement began in earnest in the 1960s, championed by the Kennedy family, in honor of Rosemary, President John F. Kennedy’s younger sister, who had an intellectual disability made worse in her 20s by a lobotomy.
A 1966 photo essay called “Christmas in Purgatory” documented terrible living conditions in institutions across the country. Geraldo Rivera, then an investigative reporter for ABC, broadcast an infamous exposé of Staten Island’s Willowbrook State School in 1972 that drew national attention to the conditions at such facilities.
Nothing was easy
Cynthia Elliott understands the history better than most. She lived it.
The eldest of four children growing up outside of St. Paul, Minnesota, in the 1950s and ’60s, Elliott’s youngest sibling was born with craniosynostosis. The bones in her skull fused too early, most likely causing brain damage. Jeannie Elliott never walked, talked or sat up. Swallowing was a challenge, which made mealtime tough.
The truth is, nothing was easy.
Their mother insisted on keeping Jeannie at home with the family, but with no services at all, she became exhausted.
“My mom was hospitalized with a nervous breakdown, and the doctor said they wouldn’t discharge my mom until my sister was gone,” Elliott said.
So at 5, Jeannie was sent to live at Cambridge State Hospital. Elliott remembers making the 45-minute drive with her family every other Sunday to visit.
“It was horrible,” she said. “That was back in the day where you’d see people walking around in hospital gowns. They didn’t have clothes.”
Because of her fragile medical condition, Jeannie lived in the infirmary. And she did have clothes. The Elliott family made sure of it.
Later she was moved to a group home where she lived for her remaining 18 years. Jeannie’s caregivers took her out for manicures and massages. They brought her to a bookstore to listen to music, and if she responded to a CD, they bought it. When the weather was good, she spent time outdoors.
“We learned that we needed to call first. Not because it was, you know, you needed to give them a warning, but because they might not be there,” Elliott said. “I mean, as severely disabled as my sister was, they were gone all the time doing stuff.”
That’s what Elliott thinks about when she checks the cameras and sees her daughter asleep on the couch in the middle of the day, her caregivers staring at their phones.
After college, Elliott worked as a special education teacher at Faribault State Hospital and then in public schools when she moved to Arizona in the mid-1980s.
When their biological daughter was grown, Elliott and her husband decided to take in a foster child, and because Elliott knew basic sign language, she and Edwards were a good fit.
Elliott has had to fight for Edwards from day one.
Related story
Schools target students with disabilities for discipline ‘too often’
These days, when she’s not monitoring her daughter’s care or providing it herself, Elliott writes to bureaucrats, testifies before the state Legislature, and files complaints with agencies like the U.S. Department of Health and Human Services’ Office of Civil Rights, which upheld her claim that the state of Arizona was violating the Americans with Disabilities Act by refusing to provide ASL interpretation for Edwards.
Elliott is now filing another complaint with the assistance of the Arizona Center for Disability Law, because she said the state failed to provide Edwards with a day treatment program for two years. She said she spent more than a year and a half trying to get the state to approve a behavioral treatment plan that her daughter’s caregivers can follow.
And then there are the near-constant calls to police. For several years, when Edwards had a seizure, she would often become combative immediately afterward. Her staff do not have permission from the state to hold her down, even for the three seconds her mother said it takes for a nurse to administer a nasal spray. So often someone would call 911.
Elliott said that lately, Edwards has gotten better at tolerating the medication with minimal intervention.
Elliott and several other family members of people with intellectual and developmental disabilities have met with Nancy Barto, a conservative Republican state senator from Phoenix.
“It really brings it home when you spend time with these families and they go into so much detail,” Barto said. “It’s extremely troubling to me that it’s continuing…If they qualify it’s the state’s responsibility to provide that service. When we fail repeatedly then things have to change.”
With the help of Elliott and other family members, the disability community had several wins during the legislative session that ended in June.
Barto helped secure more funding than has been made available in many years to pay caregivers, although lobbyists for the direct service provider industry estimate there is still a shortfall of more than $120 million.
All state employees in Arizona received a 10% raise, which is significant because support coordinators for the Division of Developmental Disabilities had not received one in a decade.
Perhaps equally important, the Arizona Legislature passed several measures that – if implemented properly – could increase oversight and accountability in the state’s system, including:
*Funding of $1.2 million for a three-year pilot program to conduct an independent review of group homes.
*An increase in the number of Adult Protective Services investigators, as well as funding for an audit of APS.
*The addition of “emotional abuse” to the list of abuse categories that Adult Protective Services can investigate.
*A new law allowing guardians to have cameras placed in common areas of a group home at the guardian’s expense.
“It’s extremely troubling to me that it’s continuing. … If they qualify it’s the state’s responsibility to provide that service. When we fail repeatedly then things have to change.”
Nancy Barto, an Arizona state senator
In testimony earlier this year before the state Senate Health and Human Services Committee, which Barto chairs, Elliott described the experience of meeting with the senator and other families.
“When we started to meet with you, Senator Barto, I was surprised that all of us as parents felt that our kids are so unsafe, that we wish that we would pass away with our children,” Elliott said. “I was shocked that there were others that have the same fear that our children’s safety and well-being is jeopardized by living in a DDD group home.”
“Grand Canyon of service gaps”
It’s not just about pay increases and better oversight. There is a fundamental disagreement within the disability community over how best to provide services to people with the most complex needs.
The federal government has changed guidelines on home- and community-based services to broaden the definition of acceptable housing to include some larger facilities as well as remote settings such as farms, but there is a heated debate in the disability community about how best to serve people with the most complex needs, many of whom have autism.
Jill Escher lives in northern California and heads the National Council on Severe Autism, an organization that is controversial for many reasons – including its name. Her son, now in his 20s, is autistic and lives in a house with support staff in the community close to his parents, who see him daily. The home has locks on the doors that can be used to prevent him from wandering. Many advocates in the disability community are opposed to any kind of locked living environment. Escher said it’s required for safety.
“Society basically wants nothing to do with my son,” she said. “It’s very easy for people in the disability rights community to talk about inclusion. For other people, having specialized supports is absolutely the paramount goal.”
Julia Bascom, executive director of the Autistic Self Advocacy Network in Washington, D.C., understands that the needs of people on the autism spectrum can vary dramatically. But she believes that just about everyone can live in the community. She said she’s seen it, but admits it’s somewhat rare.
“I haven’t seen it scale effectively to a state or a series of states,” she said.
Almost always, a person having behavior issues is responding to something negative in their environment. Remove that, and the behavior improves, Bascom said.
She acknowledged that it is difficult.
“It’s not just putting a group home in a neighborhood, but actually supporting that person to have relationships,” she said. “Even when we’re spending a million dollars, we’re not necessarily spending it on things that work.”
Instead of the term “severe autism,” Bascom and others in her circle prefer that the individual be described with specifics – for example, as having “complex behavioral needs.”
The conversation gets tricky, fast.
Last year, David Axelrod, who served as a senior advisor to former President Barack Obama, wrote an op-ed for the New York Times about his daughter, who has complex needs and lives in an institution-like setting in Chicago. He was vilified by the disability community because he was seen to be supporting institutionalization.
But even settings like the one Axelrod’s daughter is in sometimes won’t accept a person with aggressive behavior.
“Someone called it the Grand Canyon of service gaps,” Escher said. “That’s right. That’s exactly what it is.”

One family in California has found a way to fill that gap.
On a clear, sunny day in November 2021, Joaquin Carson waited patiently for his favorite lunch, a hamburger. Seated in the back of a car just outside of his home in the mountains east of San Diego, he was strapped into a harness for safety.
Joaquin’s sister Diana poked her head in to say hello. He smiled.
She’s his older sister but just by a year, so Diana always felt like she and Joaquin were twins. But their lives have always been different.

At 2, Joaquin was diagnosed with autism. Diana, who teaches a disability studies course at San Diego State University, said that in the early ’70s, autism was still called “refrigerator mom syndrome,” blamed on cold, insensitive mothers.
Their mother was the opposite, recalled Diana. Her parents mortgaged their home to build a swimming pool for therapy. No one wanted Joaquin to leave home, but by the time he was a teenager, his behavior was putting himself and others in danger.
The whole family piled in the car and drove Joaquin two hours to Fairview State Hospital. His mother wore black for a year. He later moved to a group home, but then developed aggressive behaviors.
“I believe he was communicating that something was wrong at home, in his group home,” Diana said.
Joaquin was sent back to the state hospital.
“There’s no humanity in that kind of a situation,” Diana said.
Ultimately, Diana decided to take Joaquin home.
She and her husband purchased a home with a barn an hour east of San Diego. The barn was retrofitted or, as Diana put it, “Joaquinified,” to make it safe for him and his caregivers. Diana has an office upstairs.
At first, a virtual tour of Joaquin’s home is jarring. It’s bare — the refrigerator bolted to the wall, the television behind plexiglass. The windows are shatterproof. There’s no furniture that can be thrown; even a toilet lid can be dangerous. Joaquin’s room holds little more than a bed frame and mattress. But there are homey touches like murals, an alternative to artwork hung on the walls.

Diana said they’ve been lucky to have staff that has stuck around for years.
Brittany Merrill, who has worked with Joaquin for the past eight years, said she is the lucky one.
She’d worked different jobs, including head cashier at Home Depot, but Merrill felt called to work with people with developmental disabilities.
“My sister is special needs, she’s developmentally delayed, and I have always been a part of that and caregiving for her and I cared for my grandmother till she passed away,” she said.
Merrill said she works closely with Joaquin’s sister, as well as the agency that hired her. She received training on how to work with someone who is having a seizure, as well as people with complex behaviors. There is ongoing training on how to use a letter board, a device Joaquin uses to communicate.

The team of people who care for Joaquin – including a coordinator, behavioral therapist, nurse and caregivers have monthly meetings.
Merrill makes $18.50 an hour. And the work can be difficult.
“These jobs, they are mentally draining. You just have to make sure you take the breaks you need and try not to get overwhelmed because you will have those days that are harder than others.”
But she said it’s worth it.
“Our team – we are one big family,” she said. “And once you have those dynamics you don’t want to give up.”

Though he doesn’t say much, those close to Joaquin said they believe he is happy. When the family was struggling to get him out of the institution, she recalled, their mother asked him what he wanted her to make for him to eat when he got out.
“Steak!” was the answer, which confused Diana, who doesn’t recall eating it growing up. To this day, she said, if Joaquin is having a good day he’ll announce, “I like steak.”
He loves anything on wheels, his sister added – bikes, motorcycles, cars.
So a car ride to get a burger is a pretty good thing.
Diana is grateful their mother knew Joaquin was in a good place before she died in 2015. She said she knows Joaquin is lucky, that they’re all lucky to have a close family who support one another, that she and her dad were able to draw from retirement savings to retrofit the barn for Joaquin, and that she’s able to be close by.
What about others?
“That’s the million dollar question,” she said.

Joy in small victories
On a pretty winter day in Mesa, Arizona, Zainab Edwards made a brief appearance at the park near her house. She wore a harness designed to keep her safe when riding in the minivan necessary to transport her entourage, who trail behind. After a few minutes, Edwards was ready to go home. She didn’t want to talk to a reporter, looking away shyly.
The van pulled away and Cynthia Elliott – who drove separately – found a shady spot at a picnic table. She spoke about her sister Jeannie’s life, about her own time teaching special education, about what Zainab’s life was like before the autoimmune encephalitis.
Since she got sick, every single thing seems to be a struggle.
Recently, Elliott said, “I was changing her ostomy bag. And they [the staff] had let it leak all night so her skin was really raw and so it hurts.”
After that, Elliott demanded 24/7 nursing care for Edwards. The state agreed. Elliott credited the behavioral coach, nursing care and the cameras – which she monitors constantly on her phone – with keeping Zainab safe. But the trips to the emergency room continue. Elliott was not sure how long this can go on and lately, she said, she’d started to wonder if an institution wouldn’t be a better option for her daughter.
“Some facility that could safely provide for all of her needs,” Elliott said.
Shortly before the pandemic, Elliott and several other local advocates drove to the tiny town of Coolidge, to tour the Arizona Training Program. They wanted to see what an institutional setting looks like. The expansive grounds once housed more than a thousand people, but today only a few dozen remain. When the last person dies, it will close.
Elliott recalled that the other advocates — most of whom have family with intellectual or developmental disabilities – were shocked at the setting. She was not.
“I have some comparison and I thought it looked pretty good,” Elliott said.
If the institution was still accepting new people, Elliott would probably send her daughter there, she said, looking wistful. She’s not sure Edwards will be safe anywhere in the community.
“I get that Zainab is difficult and she doesn’t fit anywhere.”
Elliott isn’t giving up. For now, she is trying to find joy in small victories.
“We’ve reached the point of really exhausting medical options and really, really focus on the positive days we have and enjoy the activities we can do with her and the community,” she said.
This past summer, Edwards took part in a couple of skating exhibitions, taking the ice in a Cinderella dress complete with a tiara and white lace gloves. Some days seizures keep her off the ice; other days she’s able to cross the ice with help.
“Anything we can do that’s something she is passionate about, we let her do it, as limited as it might be. It doesn’t matter,” Elliott said. “She counts the months till the next skating exhibition. She’s already talking about that.”
Clarification: Dec. 22: An earlier version of this story said that Jill Escher’s son lived in a gated community. He lives in a house in the community, which has locks on the doors that can be used to prevent him from wandering.



