Updated May 16, 2024
The Mental Health Parity Collaborative is a partnership between The Carter Center’s Rosalynn Carter Fellowships for Mental Health Journalism, The Center for Public Integrity, and news outlets in Arizona, California, Colorado, Georgia, Illinois, Oklahoma, Tennessee and Texas. More than 40 reporters and editors from more than 15 news outlets are working to produce data- and solutions-driven stories that examine access to mental health care in their states and why mental health parity hasn’t been achieved. Check out the latest stories below, along with those from the previous collaborative cohort.
Background
In 1996, the breakthrough Mental Health Parity Act was passed — the first legislation to require that certain insurance providers cover mental health benefits the same, or on parity, with medical benefits.
By the numbers
- More than 1 in 5 U.S. adults experience mental illness each year
- More than half of U.S. adults with a mental illness — 27 million people — don’t receive treatment—a number that has been on the rise since 2011
- Roughly 1 in 10 people who struggle with mental illnesses have no health insurance
- 60 percent of children experiencing major depression are not receiving care
Yet even after the Mental Health Equity and Substance Abuse Parity Act passed in 2008, expanding the reach of the 1996 law, along with the Affordable Care Act in 2010, parity between mental health care and medical health care is far from being achieved. Millions of people struggle to find, receive, and afford appropriate mental health treatment and, as a result, are forced to pay out-of-network costs or not receive care at all.
Though stigma still shrouds awareness of mental health issues, they are pervasive and have serious implications, putting people at high risk for suicide and crisis. This situation was exacerbated by the Covid-19 pandemic, with data indicating increased rates of depression, anxiety and suicidal ideation. At the same time, we face a national shortages of counselors and therapists.
Want more information?
Interested in connecting with us or learning more about mental health parity? Email Nora Fleming at Nora.Fleming@cartercenter.org.
FEATURED STORIES

Despite efforts to close gap, parity in mental health care remains elusive
Newsrooms in nine states reported on disparities in mental health treatment and efforts in some states to improve access. (From Center for Public Integrity and Carter Center)

Families take drastic steps to help children in mental health crises
An insufficient mental health care system pushes some families to give up custody of their children for care. States look for better solutions. (From the Center for Public Integrity)
OTHER STORIES

The Often Vicious Cycle Through SF’s Strained Mental Health Care and Detention System
Dispatchers received at least 24,000 calls about mental health crises last year. Often, responders couldn’t find the people in distress. (From San Francisco Public Press)

You Report an Unhoused Person in a Mental Health Crisis. This Is What Happens Next
Reporters spent months investigating how people can be detained involuntarily due to mental health crises and what happens to them afterward. (From San Francisco Public Press)

Oklahoma sends a growing number of kids with complex needs out of state for treatment
The state lacks options for kids with developmental disabilities and mental health needs. Oklahoma spent more than $5 million to send 49 kids out of state for treatment in the past year. (From The Frontier)

When children are rushed to the hospital in Memphis, trauma counselors are there waiting for them
Since January 2021, Le Bonheur has been providing free, trauma-informed mental and behavioral health services to more than 3,000 children admitted to the hospital for unintentional traumatic injuries. (From Institute for Public Service Reporting)
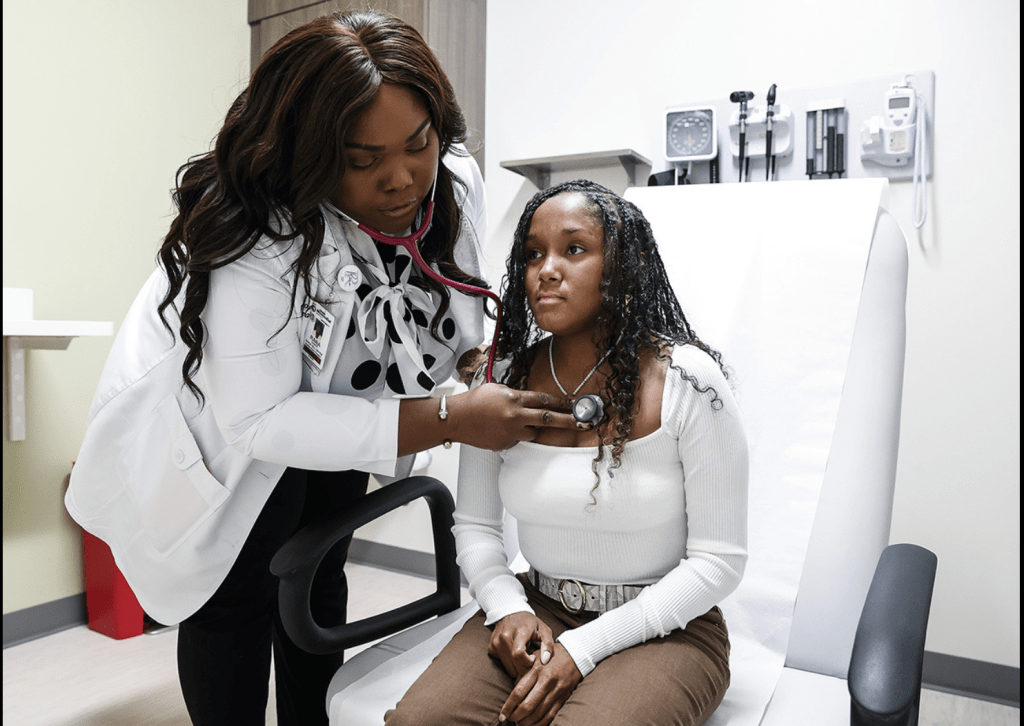
For many Black sickle cell patients, care must reach deeper
In Memphis, Black patients with an inherited blood disorder carry trauma from the dismissal of their chronic pain and severity of their symptoms. (From the Daily Memphian)
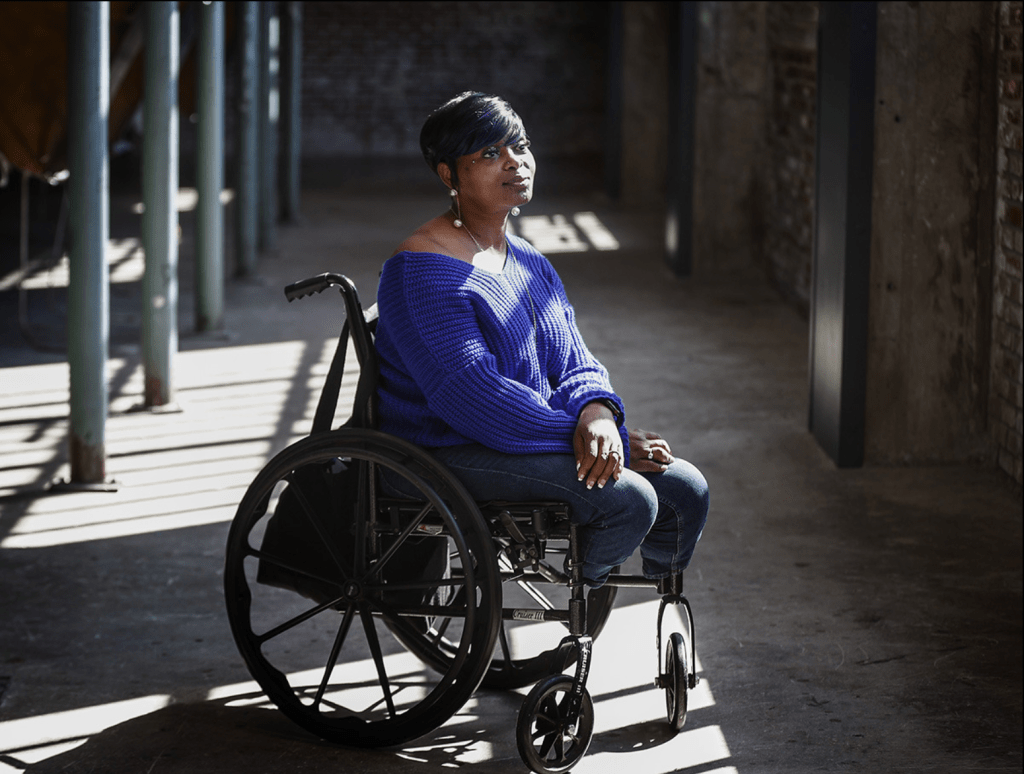
Mental health issues complicate treatment for sickle cell patients
Sickle cell disease patients’ negative experiences lead to medical mistrust, overall health disparities and mental health conditions like depression and anxiety. (From the Daily Memphian)

More options, less stigma: How Georgians in recovery are breaking barriers to addiction care
For people living with addiction, it’s been proven that access to evidence-based treatment and support can help keep them alive and stable. But care can be hard to come by and is only possible by combating the stigma around addiction, which is pervasive. (From GPB)
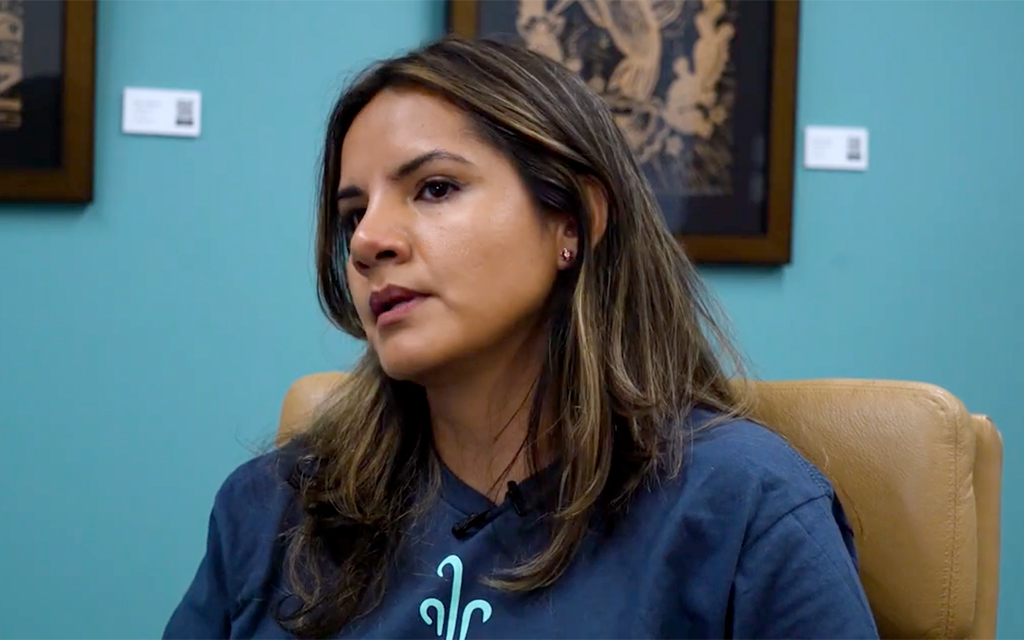
In Arizona, advocates say anti-immigrant policies have fostered a culture of fear that prevents undocumented immigrants and DACA recipients from accessing the mental health care needed to address the anxieties caused by those same policies. (From Cronkite News)

Fort Worth charter school focuses on trauma-informed curriculum. What does that mean?
Nationwide, almost 1 in 5 students between 12 and 17 reported experiencing physical assault, and about 2 in 5 reported witnessing violence, according to the Substance Abuse and Mental Health Services Administration. But not all trauma in a child’s life is so obvious. (From Fort Worth Report)

Here are the ways Fort Worth schools provide mental health care to students
School districts in Fort Worth use Communities In Schools as part of their toolkits to care for students’ well-being. They also offer counselors, telemedicine options and programs tailored to meet the specific needs of students. Research shows that Students whose mental health needs are addressed tend to perform better in school. (From Fort Worth Report)

She called the number on her syllabus offering counseling. No one picked up.
Like a lot of students, Isabelle Dizon was looking for mental health support. Her college promised to help but never came through. (From WBEZ)

Deadly Failure: A Sailor Was in Crisis. Her Command Kept the Pressure on Anyway
Together, the thousands of pages of documents and hours of interviews say one thing clearly: The treatment Tiara Gray received in the Navy played a role in her death. (From Voice of San Diego)

How the Texas vision for seamless mental health care fell apart over 60 years
A lack of private providers, a swamped community mental health system, and low insurance reimbursement have cut off many in Texas from basic mental health services. (From the Texas Tribune)

Oglethorpe County residents face barriers to mental health care, even as teens and schools are willing to have the conversation. (From UGA/The Oglethorpe Echo)

Poor access to mental health care leaves Georgia children who need a psychiatrist in the lurch
As mental health conditions rise among children, public schools are sometimes the first and best option for early intervention — especially in Georgia, where health care shortages are worsening and broadband access is not widespread. (From GPB)

Colorado’s quiet killer: Alcohol ends more lives than overdoses, but there’s been no intervention
In this four-part series, The Denver Post investigated why so many Coloradans are dying from drinking, and what the state could do in an effort to reduce the number of people lost. (From The Denver Post)

Being ‘my own role model’: Normalizing mental health care in the AANHPI community
For members of Asian American, Native Hawaiian and Pacific Islander communities, seeking mental health care can involve not just disclosing personal information, but also negotiating language barriers and cultural stigma. (From Cronkite News)

AHCCCS alerted to ‘predictable’ homelessness surge before fraud crackdown
The state agency at the center of Arizona’s ongoing behavioral health crisis knew its proposed billing reforms could trigger a surge in homelessness nearly a year before implementing the changes, yet still failed to adequately prepare for the fallout—or adjust its response to the crisis that emerged as a result. (From AZCIR)

Suffering in silence: Male college students less likely to seek counseling
Only 22.5% of male undergraduate students received psychological or mental health services over the course of a year, compared to 39.5% of female students and 63.3% of transgender and gender-nonconforming students.(From the AJC)

These Oklahomans Needed Mental Health Care. Instead, They Died in Jail.
Across the state and country, families can’t access sufficient mental health care for their loved ones and turn to police for help in a crisis. With law enforcement involved, emergency situations can escalate quickly, leading to arrests and incarceration in jails where detention officers with minimal training are responsible for the health and safety of detainees. (From Oklahoma Watch)

GOP-led push to fund police over counselors leaves some schools ‘in the lurch’
District and charter schools requested funding for hundreds of counselors, social workers and campus officers, citing problems with bullying, trauma, suicidal ideation, truancy and more. About a third of mental health positions went unfunded after the grant program ran out of cash. (From AZCIR)

The mental health of migrants simmers below the surface as the next looming crisis
WBEZ interviewed more than 30 people to understand the emotional toll migrants face, the army of helpers who are filling in the gaps of a frayed mental health system, and what’s at stake. Some of those helpers’ efforts are catching the attention of leaders in other big cities where migrants are heading. (From WBEZ)

From long wait lists to high costs, finding a therapist in Colorado is harder than it should be
In communities across Northern Colorado, people are struggling with their mental health while also struggling to get the care they need. (From KUNC)

Law Could Increase Demand for Often-Elusive Addiction Treatment
A state law set to take effect in January aims to make it easier to force Californians with severe substance use disorders into treatment that is now often not immediately available to San Diegans who want it. (From Voice of San Diego)

Patients, advocates describe ‘pure chaos’ in state response to AHCCCS fraud
Arizona’s failure to adequately anticipate the impact of widespread suspensions among behavioral health providers due to fraud has put an already susceptible population at further risk of relapse, abuse, homelessness and even death as operators shut down. Advocates—and the providers left standing—are struggling to meet the urgent need for services among displaced tribal members and other victims. (From AZCIR)

One answer to the youth mental health crisis? Asking Colorado students how they’re feeling
Rates of anxiety and depression among young people are the highest they’ve been since 2013, when Colorado first began collecting this data. Driven by the urgent state of youth mental health, an effort is underway in Colorado to identify kids who need behavioral health help before they are in crisis. (From KUNC)

Overwhelmed with mental health calls, six rural sheriffs make their own plan for better response
Law enforcement are often the first and only ones who respond to calls when people have a mental health crisis, especially in rural areas where behavioral health providers are lacking or completely unavailable. (From GPB News)

Getting drug treatment beds is so hard for poor it’s like winning the lottery
Low-income and homeless San Diegans often can‘t quickly access residential treatment for substance use disorder. Only two detox beds for Medi-Cal patients are in the city of San Diego, which until recently had no beds for these patients. (From Voice of San Diego)

Cover-up Alleged in Pottawatomie County Jail Deaths
Pottawatomie County jail officials apparently defied state laws and a judge’s order when they concealed information on the unexplained deaths of seven vulnerable detainees. (From Oklahoma Watch)

This Harris County program serves the most vulnerable. But it won’t bail them out of jail.
The Harris County Jail has continued to struggle with caring for an influx of inmates with mental illnesses. Many of the inmates who died in custody hadn’t received desperately needed care.(From Houston Landing)

There have been nine suicides at the Oklahoma County jail in three years. Another six people with documented mental health issues died of other causes. One woman’s death has helped jumpstart a diversion program. (From The Frontier)

LGBTQ+ kids in Colorado are struggling. Finding the right therapist is yet another hurdle
Colorado’s LGBTQ+ youth are living with high rates of depression, stress and thoughts of self-harm, but finding treatment in Northern Colorado can be a challenge. (From KUNC)

Mental Health Care Is Critical for Survivors of Violence. Access Is Another Story
Californians in general struggle to find and afford mental health treatment, but the access difficulties are magnified for survivors of domestic violence. (From California Health Report)

How San Diego Is Rolling Out CARE Court
San Diego County is up against the clock to implement a new state-mandated system that compels people with certain mental illnesses into care. It’s a herculean task, and one with many obstacles. (From Voice of San Diego)

Proven Schizophrenia Treatments Keep People in School, at Work and off the Street. Why Won’t Insurance Companies Cover Them?
Treatment programs recommended by the National Institute of Mental Health as the gold standard of care for early psychosis rarely have enough slots available for the people who need them, and health insurance companies typically refuse to cover the full cost of these programs. (From KQED)

Jails fail to accommodate people with mental illness. In some cases, it’s a civil rights violation
Conditions in some corrections facilities are a moral failure that also costs taxpayers millions.
WITF found that nearly one-third of so-called “use of force” incidents with pepper spray, stun guns and other distressing methods of control involved a person with a serious mental health issue. (From WITF)

Uvalde prompted Texas to start taking mental health in schools more seriously. Is it enough?
The May 24 shooting at Robb Elementary school in Uvalde, Texas, that killed 19 children and two teachers pushed several important issues into the national conversation, including the availability of guns, school security, and mental health access. (From Texas Public Radio)

Texas bans many proven tools for helping drug users. Advocates are handing them out anyway
As overdoses skyrocketed amid the pandemic and the fentanyl crisis, advocates across the state are working discreetly to distribute these supplies as part of a practice to combat substance use disorder known as harm reduction. (From The Texas Tribune)

California is trying to house the homeless through a health insurance program. It worked for this man.
At the beginning of the year, California began rolling out extensive reforms to Medi-Cal, the state and federally funded healthcare program which serves low-income adults and children. (From The Los Angeles Times)

Healing through culture: Increasing access to Native American practices to treat mental health
Researchers have long pointed to the importance of incorporating cultural practices into behavioral health care for Native Americans, but there is an ongoing struggle to ensure those services are accessible and affordable. (From Cronkite News) Related Indigenous healing: A documentary

“It’s destroying me”: Storm after storm, climate change increases strain on Texans’ mental health
Tens of thousands of coastal Texas residents have survived repeated extreme weather events including Hurricane Harvey. For many, it has taken an emotional toll, and researchers warn that climate change could be “catastrophic” for our mental health. Related podcast. (From The Texas Tribune)

There’s Free Mental Health Help For Crime Victims, But Providers Say Bureaucracy Gets In The Way
Therapy sessions were covered through a program administered by the California Victims Compensation Board, which reimburses crime-related mental health expenses. But process changes and ongoing bureaucratic slowness with CalVCB has made serving crime victims more difficult than ever. (From LAist)

In March 2020, Gov. Doug Ducey signed into law a sweeping set of measures designed to help curb rising rates of suicide and expand access to mental health treatment for Arizona residents with and without insurance.Yet, two years into the program, more than half of Arizona schools haven’t referred students under the law. (From AZCIR)

A new national mental health crisis line launches soon. Some states aren’t ready
The new crisis line is expected to send call volume soaring, and that means states like Illinois have a tough hill to climb. (From Side Effects Public Media)
- Listen to a discussion about the new mental health crisis line on NPR’s Morning Edition.

Why is it so hard to find therapists who take insurance in Illinois?
Many mental health professionals no longer take health insurance because they say they’ve grown frustrated with insurance companies not paying them enough, taking too long to pay and making them jump through hoops to give patients the care they need. (From Chicago Tribune)

How researchers are getting farmers to talk about mental health
A survey of farmers and farm workers in Georgia painted a startling picture. Farmers living a brutal reality of isolation and loneliness. A persisting dissatisfaction with their jobs while struggling to manage stressors like extreme weather and hiking supply prices. (From GPB News)

Farmers have silently struggled with their mental health for years. Are they ready to talk?
The fallout of Hurricane Michael in 2018 and the chaos caused by the pandemic shed light on a problem that, until recently, has only been discussed in hushed tones behind doors: the deteriorating mental health of Georgia’s farming community. (From GPB News)

It’s the most important part of addiction recovery — and often the most difficult to access
Medical detox, inpatient rehabilitation and ongoing counseling are often not paid by insurance, even when patients have coverage. Many substance abuse counselors don’t even accept insurance. (From GPB News)

CARE Court Aims To Help People Living With Serious Mental Illnesses.
There’s a bill making its way through the state legislature that aims to create new avenues for people living with a serious mental illness to get life-saving treatment. (From LAist and KPCC)

Why The Pandemic Took An Especially High Mental Health Toll On New Parents
Between February and July of 2020, one in three birthing parents experienced postpartum depression, up from one in eight before the pandemic. (From LAist and KPCC)

The state ranks at or near the bottom on several key indicators of youth well-being, such as the percentage of kids with untreated depression. (From AZCIR)

For trans youth in North Texas, finding affirming mental health care can be a challenge
Texas leaders have targeted trans youth, their families and gender-affirming care practices for months. (From KERA)

With few other resources, people with behavioral health issues find treatment in jails and prisons
Jails are the state’s de facto mental health facilities. (From Georgia Public Broadcasting)

Amidst a lack of mental health services, the ‘Living Room’ approach aims to plug gaps
Living Rooms offer an alternative to the emergency room and jails, which often become the default providers of emergency mental health care. (From Side Effects Public Media)

The law governs assisted outpatient treatment, or AOT, a court-ordered treatment plan. Standards to qualify for AOT are lower than those needed for an involuntary 302 hospitalization. (From PublicSource)

Georgia students’ private battle: Anxiety disorders in the classroom
“We’re putting our kids in these incubators of pressure,” said licensed psychologist Josh Spitalnick of Anxiety Specialists of Atlanta. “(It’s) not surprising that we’re seeing more families in a clinic like ours.” (From The Atlanta Journal-Constitution)

Law enforcement enlists mental health experts to help save lives — ‘a paradigm shift in policing’
It’s a change from previous tactics when people suffering from mental crises were often arrested, a strategy that only exacerbated their issues and resulted in jails filling up. (From Georgia Public Broadcasting)

PA eased telehealth regulations during the pandemic. What happens if the waiver expires?
The unprecedented access to telehealth was appreciated by many patients and doctors, like the patients receiving physical therapy without leaving home and doctors seeing more patients in a day and managing those more effectively. (From PublicSource)

During the pandemic, many Chicago organizations began rethinking how to provide mental health help as the virus swept into the city. (From Chicago Tribune)
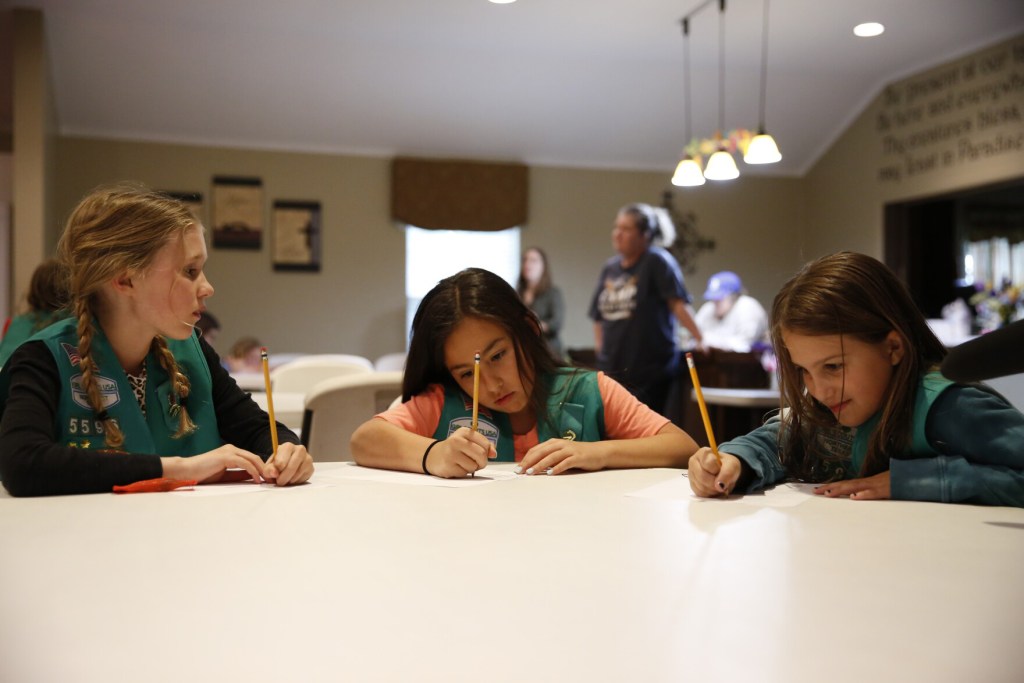
The Girl Scouts of Northeast Texas are tackling mental health, one patch at a time
The COVID-19 pandemic worsened stress, anxiety and depression for young people—especially young girls. (From KERA)

CREDITS
Project manager and editor: Nora Fleming
Editors: Jennifer LaFleur and Matt DeRienzo
Designer: Janeen Jones
Audience and engagement: Lisa Yanick Litwiller and Vanessa Freeman
PARTNERS