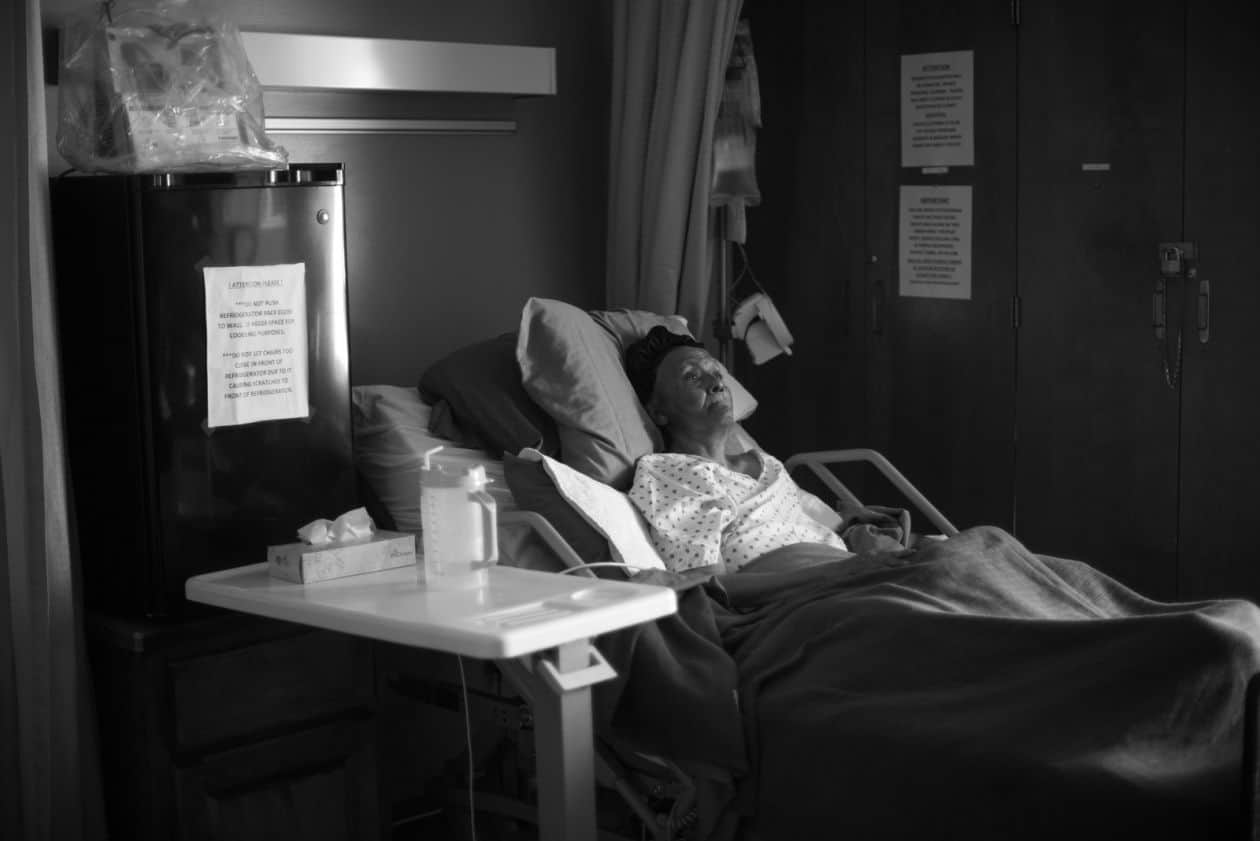
In 2009, while at The Chicago Reporter, I took a deep look at racial disparities in the quality of care in nursing homes in Chicago, Illinois and nationally. For a project that the Center for Public Integrity published in November 2014, I brought together Medicaid cost reports, self-reported staffing figures, testimonies from advocates and lawyers, and personal stories from nursing home residents and their families to address a simple question: how much care is a loved one actually receiving at a nursing home? The conclusion? Nursing homes serving minorities offer a lot less care than those predominately housing whites.
Story genesis
The three-part series began with a leftover.
Toward the end of my reporting on The Chicago Reporter story I brought together self-reported staffing levels on Nursing Home Compare, a government website the public uses to compare and evaluate nursing homes, with the average daily levels of care I calculated by looking at Medicaid cost reports.
I found that the self-reported data was higher than the daily figure from the cost reports in many more than half of the facilities.
Intrigued, I spoke to advocates and lawyers who said the finding suggested that nursing homes “staff up” for inspections.
Toward the end of 2013 I submitted FOIA requests for four additional years of Illinois cost reports. I repeated the analysis and found similar results that convinced me the first year was not an aberration.
David Donald, then the data editor at the Center for Public Integrity, encouraged me to locate cost reports for all 50 states in order to tell a national story.
Finding the data
Fortunately, the website for the Centers for Medicare and Medicaid Services (CMS) had this information as the Affordable Care Act required that all skilled nursing facilities submit cost reports.
But finding the data presented a real challenge as the first person with whom we interacted told us that the data we wanted was not kept in the cost reports. We looked through the nearly 100-page data dictionary before we found that was not true.
From there we needed to tackle the data.
At more than 14 million records, the file was the largest I had ever analyzed. It took me days before I could connect the data fields with their corresponding values in the dictionary.
I filtered the data with statistical software SPSS before getting a quantity of them I could analyze in Excel.
I located a 2007 peer-reviewed paper about over-reporting of staffing levels in Texas nursing homes. Guided by lead author Bita Kash and assisted by Charlene Harrington, a longtime national authority on nursing home staffing, I conducted the national analysis of more than 14,000 nursing homes.
Crunching the data
The analysis took weeks. Guided by our desire to find out if the gap we had identified in Illinois between self-reported staffing levels and the average daily level we found through the cost reports was national, we used Access to bring together the data sets, Excel to perform a preliminary analysis and SPSS to determine if we found had any statistical basis.
The gap was systematic, cutting across all ownership types, geographies and positions. Among the three direct care positions of certified nursing assistant, licensed practical nurse and registered nurse, the latter stood out by far.
More than 80 percent, or about five in six nursing homes, had higher registered nurse staffing levels on Nursing Home Compare than the daily average we calculated through the cost reports.
For more than 25 percent, the Nursing Home Compare figure was at least double the one we calculated through the cost reports.
These staffing discrepancies mattered for a number of reasons. They suggested that what a potential consumer thinks their loved one will receive in daily care is often much higher than the actual daily level of care. The discrepancies happened after more than a decade of reports and documents from CMS that said repeatedly that self-reported data from nursing homes are inaccurate. They come at the beginning of the “silver tsunami”, the explosion of aging Americans who could need that nursing home care. They also occurred at a time when the number of standard survey inspections dropped each year from 2008 to 2012, falling six percent during those years. The number of nursing homes decreased just one percent in the same period.
Less government attention only heightened the importance of having accurate data, advocates said. Beyond all that, a provision of the Affordable Care Act required that nursing homes transition from using self-reported to payroll-based data by March 2012. But in late 2011 the agency said it needed more time to implement the provision.
Little had happened since.
We subsequently used SPSS, Excel and Access for a separate story that identified and sought to explain national disparities in the amount of registered nurse care in nursing homes where most residents are black or Latino compared with those where the majority of residents are white.
During this part of the process we spoke with advocates, industry figures, academics and lawyers to identify and find data for as many different variables as possible that could possibly explain these disparities. We did this because we wanted to rule out any other possible reason for the differences in registered nurse care. Eventually, we found data about the residents, the level of market competition and the area where the homes were located.
None fully explained the disparities.
Adding human stories
Critical to each story in the project was a series of conversations with people who had been directly impacted by the issues we had uncovered. We met Lisa Sanders through Martha Deaver, president of advocacy group Arkansas Advocates for Nursing Home Residents.
With the help of Deaver and the state’s Long-Term Care Ombudsman, Sanders had helped build one of the largest family councils in the state. She told us her story and introduced us to other families. All were black. All had loved ones who had spent time and experienced problems in nursing homes with extremely low registered nurse staffing levels such as dehydration, falls, urinary tract infections and sitting in soiled clothes for long stretches of time. All the people we interviewed decided that caring for their loved one became a full time job and became increasingly impatient in their interactions with facility personnel. And all articulated a poignant and painful mixture of grief, guilt, helplessness, frustration and betrayal at what they perceived to be the home’s failure to live up to its stated commitment of providing their loved one the care and dignity they deserved. Meeting and learning from these people moved us a lot and reinforced to us the vital importance of of using data and documents to unpack the impact of policy and it’s lack of enforcement on people’s lives.
Publishing the story and its interactive elements
In an effort to reach as many audiences as possible we published the full project in English on the Center for Public Integrity’s website, shorter versions of the two main staffing stories onNBCNews.com, and in Spanish at Hoy Chicago, the Chicago Tribune Company’s Spanish-language newspaper.
We also published a series of photographs on my brother Jon Lowenstein’s Instagram feed, which had close to 100,000 followers. We embedded investigative data, content and findings in the captions and dialogued with people around the world.
The Center for Public Integrity’s news apps developer Chris Zubak-Skees used Javascript to build a lookup table in which people could find staffing information for more than 10,000 nursing homes across the country.
We used Google Fusion Tables to build a map of nursing homes that received low-cost, HUD-backed mortgages the month after receiving the lowest possible rating for quality of care from Nursing Home Compare.
Impact and reflections
The project had impact on a number of levels.
It attracted widespread national media pickup in online, television, print and radio formats. U.S. Rep. Jan Schakowsky (D-IL) said it helped shape her thinking for legislation she’ll introduce this year and pledged to take action on each part of the series. The Office of Inspector General in the Department of Health and Human Services is deciding whether to take action against a Chicago-area chain. A state senator in Illinois said she plans to convene a hearing about the issues raised by the series. A pair of professors at John Marshall Law Schooland a corporate law firm are considering filling a civil rights car against a Chicago nursing home operator.
I presented the work during the plenary session of the annual conference for the National Consumer Voice, the nation’s largest nursing homes advocacy group, and spoke during a monthly conference call to more than two dozen long-term care ombudsmen from around the country. After these presentations I shared and discussed data with advocates, government agencies, long-term care ombudsmen and family members in about a dozen states.
This was the largest investigative project I’ve done so far. Conceiving, bringing it to fruition and seeing it ripple in different arenas was deeply gratifying.
But more leftovers remain.
This story originally appeared on Storybench, a new blog on digital storytelling by Northeastern University’s Media Innovation program in partnership with Esquire magazine.