Are you a health worker, medical provider, COVID-19 patient, or federal employee on the front lines of the pandemic? We want to hear from you. Email us tips@publicintegrity.org.
¿Es usted trabajador de salud o de otro servicio de primera línea, o paciente de COVID-19? Cuéntenos, en español si prefiere, de sus inquietudes a tips@publicintegrity.org.
They’re not doctors or highly trained nurses.
But legions of low-profile hospital workers — from skilled therapists and translators for non-English speakers to room cleaners and meal servers — are bemoaning their risk for coronavirus exposure.
Workers in California, Illinois and Washington state, where COVID-19 cases are numerous, tell the Center for Public Integrity they fear inadequate access to personal protective equipment that could shield them. Two nurses in New York City have died from the virus, and it’s left hundreds of other hospital workers ill.
Many hospitals are struggling to obtain the equipment and rationing what they do have.
Angst is mounting among workers because the Centers for Disease Control and Prevention on March 10 reacted to national shortages by easing guidelines on when and which healthcare workers should be prioritized for optimal gear — especially the coveted N95 respiratory masks that filter out 95 percent of small particles that may carry the virus.
There’s also meager support for low-paid hospital workers who are least able to afford to self-quarantine if exposed to the virus, said Catherine Murrell, deputy communications director for Healthcare Illinois and Indiana, a healthcare workers’ union affiliated with the Service Employees International Union.
Wellington Thomas, an emergency room tech at Chicago’s Loretto Hospital, is a worker who fears his hospital will run out of protective supplies. He worries that he won’t get paid if he tests positive and has to stop working to self-isolate.
ER techs are among the first workers to see patients. They check vital signs, record symptoms, provide physical assistance — if necessary — and aid nurses. Thomas earns a little more than $19 an hour, more than a lot of techs because of his seniority. But he only receives six days of paid sick leave per year — and only has three left for this year.
The Healthcare Illinois and Indiana union is urging hospitals to cover 15 paid sick days if a worker must self-quarantine, Murrell said.
Thomas said he’s donned adequate personal protective equipment, or PPE, if he’s called into patient isolation areas. One piece is the N95 respirator mask that hospitals are clamoring to stock. But Thomas has also been in contact with ER patients who developed COVID-19 symptoms while wearing less-than-optimal protection.
After one case of known exposure to a patient, Thomas said the hospital put his and other aides’ names on a list. “Six or seven of us were going in and out of that room all day,” Thomas said.
Administrators advised Thomas and others to monitor themselves for fever or other suspicious signs — advice that’s in line with Centers for Disease Control and Prevention guidance, Loretto spokesman Mark Walker said.
He also said the inner-city hospital, the services of which are overwhelmingly covered by Medicare and Medicaid, is “absolutely committed” to paying workers who must quarantine “if we have the funds to do it.”
Under fire for failure to provide and distribute timely aid, President Donald Trump said Sunday that new legislation will provide hospitals “critical supplies including masks,” and $2.2 trillion in relief for “families, workers, businesses and Americans of every race, color, religion and creed.”
Nevertheless, all health workers may not immediately, or ever, receive the specific protective gear they say they need now. And the federal legislation doesn’t guarantee that all healthcare workers, and workers at companies with more than 500 and fewer than 50 employees, have to be paid if put on two-weeks quarantine.
Urgent need for helmet shields in Seattle
Heather is an acute-care speech therapist in a Seattle hospital. She’s in demand to work with COVID-19 patients and worried that the hospital is running out of parts for the essential equipment she’s been using to protect herself. She asked that her last name and the name of the hospital not be disclosed because she wasn’t authorized to identify it.
As many as 60 percent of the U.S. healthcare workforce consists of people such as Heather, who are “allied” healthcare workers trained in a range of diagnostic and treatment disciplines.
Heather’s Seattle hospital is in a COVID-19 hotspot — and near to a nursing home that’s been linked to at least 37 coronavirus-related deaths.
Heather’s job, by its nature, requires her to get close to patients’ faces and look inside their mouths. She expects they’ll cough on her. She asks patients to swallow liquids or foods of differing textures to determine how well they’re breathing and swallowing as they come off ventilators.
The tests, she explained, determine if patients are “aspirating,” or breathing substances into their airways and lungs. Aspirating prevents recovery from pneumonia and can nurture new infections. What Heather does is crucial to measuring fragile patients’ condition and for designing treatment for recovery.
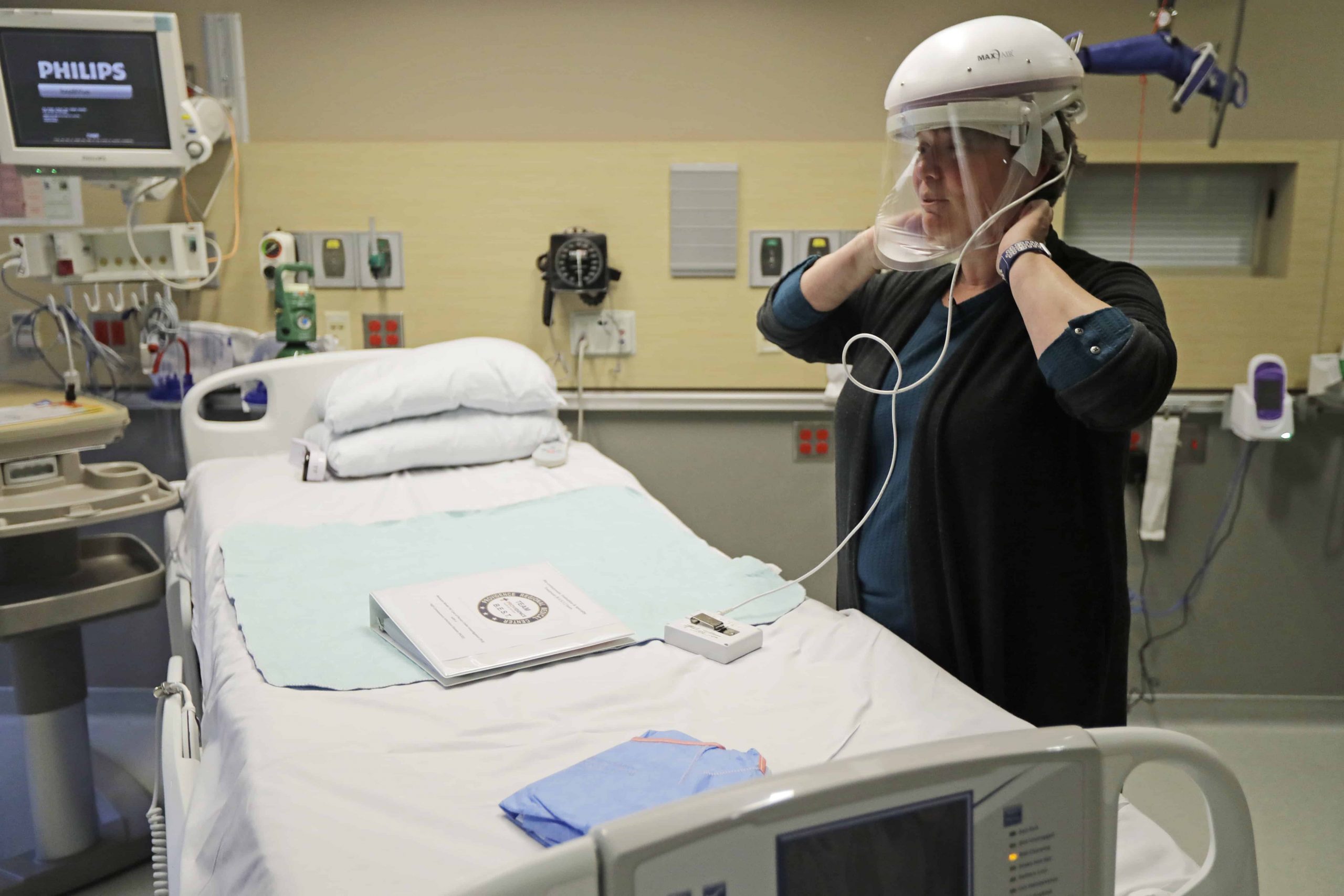
To protect herself from infectious droplets and mist, Heather has been using a CAPR — a controlled air purifying respirator. The tool consists of a helmet with a removable face shield, an air filter, a battery pack worn on the back and flexible material that creates a suction around the neck.
Nurses also use CAPR devices, but Heather said they have individual, detachable face shields assigned to them. Heather must pick from a limited supply of shields shared among workers who also perform tasks essential to patient care, which could increase the risk of infection. Those sharing shields include ultrasound technicians and lab techs who draw blood.
“There’s a table with three or four shields. You have to pick one,” Heather said. “And you have to hope the person who used it before you did a good job cleaning it or do it yourself.”
Because workers are repeatedly cleansing the shields with bleach wipes, as protocol demands, the shields are breaking down, Heather said. The material that seals the respirator is also deteriorating. Her hospital urgently needs more parts to keep the CAPRs working safely.
Because the CAPR is loud, Heather said she’d prefer to use an N95 respirator — a smaller, special facepiece that guards against airborne droplets and mist. There is a national shortage of N95s, which the Centers for Disease Control and Prevention identify as superior to a simple surgical mask. Some workers use N95s with eye protection. Many workers have only access to surgical masks. Some have no protection at all.
Heather has two N95 masks at home from a prior job, although she hasn’t been able to get a required annual check to ensure that they fit. The hospital has begun fitting new doctors and nurses for N95s, she said. But to help control the supplies of facepieces, the hospital isn’t conducting fitting tests for therapists such as Heather.
Up-close interpreting in a Chicago ER
Hospital interpreters also find themselves in risky contact with patients with COVID-19 symptoms.
An interpreter in Chicago, who works in a different hospital than Wellington Thomas, said he’s sometimes inches from the faces of patients. Some have sneezed on him. He knows he’s interpreted for patients who came to his ER and left, only to return with a confirmed case of COVID-19. He said he wasn’t authorized to identify himself or the hospital.
He walked into a room recently to interpret for another patient with COVID-19 symptoms. A doctor attending the patient had on an outfit with a face shield resembling “riot control” gear, the interpreter said.
“There I was with just a surgical mask,” he said.
The interpreter has been fitted for N95 respirators, but the hospital didn’t have one available.
The patient was being treated with a nebulizer that covered her nose and mouth. The interpreter hoped that the nebulizer would act as a shield. But the treatment is also an “aerosol-generating” procedure that can emit mist that lingers.
The weakened patient had trouble speaking clearly. “I had to get really close to her,” the interpreter said.
A supply of N95s later arrived, the interpreter said, and as long as they last, he said he’ll be asking for one when he starts his shift. Ideally, N95s aren’t supposed to be reused. But anyone who uses one, the interpreter said, has been placing them in brown paper bags with names on them to keep them for reuse. Paper bag storage for N95 masks has gone national, along with hospital workers posting photos of bags and the hashtag #GetMePPE on Twitter.
“With each passing day, people are less casual about this,” the interpreter said. “Protection goes both ways. It’s for patients and workers.”
Enrica Ardemagni, president of the National Council on Interpreting in Health Care, said she’s been fielding calls from worried interpreters, many of whom are on-call workers. The council set up online training to help interpreters temporarily transition to telephonic and video interpreting.
But “face-to-face” interpreting will still be necessary in some cases, said Ardemagni, a Spanish-language interpreter and professor at Purdue University in Indianapolis.
Disinfecting rooms, safe food service in California
In Downey, California, unionized workers at the Kaiser Permanente Downey Medical Center pushed for more protection for environmental service workers, who clean rooms after coronavirus patients vacate them.

Gabe Montoya is an emergency medical technician who typically cleans wounds, splints limbs and helps with electrocardiograms and resuscitation at the Los Angeles County hospital. One of his jobs now is to help doctors and nurses correctly put on and remove gowns, gloves and facepieces before entering isolation rooms to treat COVID-19 patients. EMTs, also clad in optimal personal protective equipment, then stand outside the rooms, watching through windows, to make sure the medical team’s equipment doesn’t tear or otherwise become compromised.
“From the very start, a COVID patient takes a lot of staff,” Montoya said.
He said he’s heard the “horror stories” about lower-paid, “marginalized” workers who disinfect hospital rooms but don’t benefit from strict safety protections. Montoya worked with management at his hospital to ensure that, when needed, cleaning staff get N95s, gowns, gloves and booties.
Most of them are Latino, and many are not fluent in English, said Montoya, who also serves as a union representative for United Healthcare Workers West, which is part of SEIU.
“To me, they have one of the more dangerous jobs. They have to go into rooms with a lot of surfaces. Everything has to be disinfected — the beds, railings of the beds, behind the beds, all the cords and the walls and the floors,” Montoya said. “Without them we don’t function.”
In emails, Montoya said he’s had to remind frontline medical workers and management: “Whatever you wore in that room, they have to wear it, too.”
“To me, they have one of the more dangerous jobs.”
Gabe Montoya, an emergency medical technician, said of cleaning staff
To help secure more protective gear, United Healthcare Workers West announced March 26 that it located a distributor with a stockpile of 39 million N95 masks. The union is arranging for hospitals in the hot-spot states of California and New York to buy the masks, at $5 each. The group also put in an order for another 1 million N95s from another supplier and found a company that said it can supply millions of face shields.
Update, 10:31 a.m. April 6: The union has confirmed that subsequent hospital efforts to obtain the N95 masks fell through, as the Los Angeles Times reported. Union spokesman Nathan Selzer said that federal Coronavirus Task Force contacted the union, “looking into problems with PPE,” and that the union provided information about the supplier. “Our role was to connect those who needed PPE with a potential supplier. Once the connection was made, it was up to those who needed the equipment to work out details like quantities, payment, delivery and due diligence on the validity of the supplies. Unfortunately, as governors, counties, hospital systems and others have learned in recent days, the supply chain for this type of equipment is fraught with problems,” Selzer said in a statement.
The Department of Health and Human Services estimates that the demands of a pandemic on the U.S. care system will require up to 3.5 billion N95 masks over a year. On March 21, Democrats in Congress wrote to HHS that only 12 million N95 masks were in the Strategic National Stockpile, and as many as 5 million may have expired.
Kaiser Permanente declined to comment on negotiations with the union, and in a statement said: “We continue to provide our staff with protective equipment that is aligned with the latest science and guidance from public health authorities. … While we currently have the personal protective equipment needed to serve our patients and protect the safety of our staff, we are prudently managing our resources and are aggressively pursuing additional supplies.”
At Stanford Hospital in Palo Alto, California, United Healthcare Workers West members negotiated with managers to upgrade protections for dishwashing staff who were fearful of coronavirus exposure.
Shop steward Juan Boza said he suggested to managers that the hospital use only paper trays and containers for patients in isolation. Nurses can discard the material in patients’ rooms. The hospital, which did not respond to a request for comment, agreed to the change, Boza said. Update, 9:26 a.m., April 1: The hospital confirmed in a statement that it’s now using disposable paper meal service for virus patients and “pursuing all channels” to keep up a supply of safety equipment for staff.
“They don’t let us use masks,” Boza said. “They say we don’t need them. Just wash your hands all the time. But don’t touch your face. That’s what they keep telling us.”