GLEN FORK, W.Va. — Across Laurel Creek and down a dirt road in this sleepy valley town is the modest white house where Steve Day grew up. For more than 33 years, it was where he recuperated between shifts underground, mining the rich seams of the central Appalachian coalfields and doing his part to help make Peabody Energy Corp. the nation’s most productive coal company. Now, it’s where he spends most days and nights in a recliner, inhaling oxygen from a tank, slowly suffocating to death.
More than a half-dozen doctors who have seen the X-ray and CT images of his chest agree he has the most severe form of black lung disease. Yet his claim for benefits was denied in 2011, leaving him and his family to survive on Social Security and a union pension; they sometimes turn to neighbors or relatives for loans to make it through the month.
The medical opinions primarily responsible for sinking his claim didn’t come from consultants-for-hire at a private firm or rogue doctors at a fringe organization.
They came from a respected household name: the Johns Hopkins Medical Institutions.
The Johns Hopkins University often receives attention for its medical discoveries and well-regarded school of public health, and its hospital recently was ranked the nation’s best by U.S. News and World Report.
What has remained in the shadows is the work of a small unit of radiologists who are professors at the medical school and physicians at the hospital. For 40 years, these doctors have been perhaps the most sought-after and prolific readers of chest films on behalf of coal companies seeking to defeat miners’ claims. Their fees flow directly to the university, which supports their work, an investigation by the Center for Public Integrity and ABC News has found. According to the university, none of the money goes directly to the doctors.
Their reports — seemingly ubiquitous and almost unwaveringly negative for black lung — have appeared in the cases of thousands of miners, and the doctors’ credentials, combined with the prestigious Johns Hopkins imprimatur, carry great weight. Their opinions often negate or outweigh whatever positive interpretations a miner can produce.
For the credibility that comes with these readings, which the doctors perform as part of their official duties at Johns Hopkins, coal companies are willing to pay a premium. For an X-ray reading, the university charges up to 10 times the rate miners typically pay their physicians.

(ABC News)
Doctors have come and gone from the unit over the years, but the leader and most productive reader for decades has been Dr. Paul Wheeler, 78, a slight man with a full head of gray hair and strong opinions.
In the federal black lung system, cases often boil down to dueling medical experts, and judges rely heavily on doctors’ credentials to resolve disputes.
When it comes to interpreting the chest films that are vital in most cases, Wheeler is the coal companies’ trump card. He has undergraduate and medical degrees from Harvard University, a long history of leadership at Johns Hopkins and an array of presentations and publications to his credit. In many cases, judges have noted Johns Hopkins’ prestige and described Wheeler’s qualifications as “most impressive,” “outstanding” and “superior.” Time and again, judges have deemed him the “best qualified radiologist,” and they have reached conclusions such as, “I defer to Dr. Wheeler’s interpretation because of his superior credentials.”
Yet there is strong evidence that this deference has contributed to unjust denials of miners’ claims, the Center found as part of a yearlong investigation, “Breathless and Burdened.” The Center created a database of doctors’ opinions — none previously existed — scouring thousands of judicial opinions kept by the Labor Department dating to 2000 and logging every available X-ray reading by Wheeler. The Center recorded key information about these cases, analyzed Wheeler’s reports and testimony, consulted medical literature and interviewed leading doctors. The findings are stark:
- In the more than 1,500 cases decided since 2000 in which Wheeler read at least one X-ray, he never once found the severe form of the disease, complicated coal workers’ pneumoconiosis. Other doctors looking at the same X-rays found this advanced stage of the disease in 390 of these cases.
- Since 2000, miners have lost more than 800 cases after doctors saw black lung on an X-ray but Wheeler read the film as negative. This includes 160 cases in which doctors found the complicated form of the disease. When Wheeler weighed in, miners lost nearly 70 percent of the time before administrative law judges. The Labor Department does not have statistics on miners’ win percentage in all cases at this stage for comparison purposes.
- Where other doctors saw black lung, Wheeler often saw evidence of another disease, most commonly tuberculosis or histoplasmosis — an illness caused by a fungus in bird and bat droppings. This was particularly true in cases involving the most serious form of the disease. In two-thirds of cases in which other doctors found complicated black lung, Wheeler attributed the masses in miners’ lungs to TB, the fungal infection or a similar disease.
- The criteria Wheeler applies when reading X-rays are at odds with positions taken by government research agencies, textbooks, peer-reviewed scientific literature and the opinions of many doctors who specialize in detecting the disease, including the chair of the American College of Radiology’s task force on black lung.
- Biopsies or autopsies repeatedly have proven Wheeler wrong. Though Wheeler suggests miners undergo biopsies — surgical procedures to remove a piece of the lung for examination — to prove their cases, such evidence is not required by law, is not considered necessary in most cases and can be medically risky. Still, in more than 100 cases decided since 2000 in which Wheeler offered negative readings, biopsies or autopsies provided undisputed evidence of black lung.
In an interview, Wheeler held strongly to his views. In his telling, he is more intellectually honest than other doctors because he recognizes the limitations of X-rays and provides potential alternative diagnoses, and he is adhering to a higher standard of medical care by demanding biopsies to ensure patients get proper treatment.
“I’ve always staked out the high ground,” Wheeler said.
The university defended Wheeler, saying in a statement he “is an established radiologist in good standing in his field.”

University officials questioned the findings by the Center and ABC, requesting extensive documentation, which the news agencies provided. After initially promising responses, officials at Johns Hopkins did not answer most questions but instead provided a general written statement.
“To our knowledge, no medical or regulatory authority has ever challenged or called into question any of our diagnoses, conclusions or reports resulting from the … program,” the statement said.
After the Center and ABC again posed questions about documents showing that judges and government officials had challenged the opinions of Wheeler and his colleagues on numerous occasions, university officials sent the same statement again.
That statement also said, “In the more than 40 years since this program’s inception, [Johns Hopkins radiologists] have confirmed thousands of cases to be compatible with [black lung].”
In some cases reviewed by the Center and ABC, Wheeler opined that an X-ray could be compatible with black lung but that another disease was more likely, ultimately grading the film as negative.
The news organizations asked the university how many times he had provided a truly positive reading; Johns Hopkins officials would not answer or clarify what they meant by “compatible.”
Judges at varying times have called Wheeler’s opinions “disingenuous,” “erroneous,” “troubling” and “antithetical to … regulatory policy,” court records show.
One judge dedicated an entire section of his ruling to the Johns Hopkins specialists. Wheeler and two colleagues “so consistently failed to appreciate the presence of [black lung] on so many occasions that the credibility of their opinions is adversely affected,” Administrative Law Judge Stuart A. Levin wrote in 2009.
“Highly qualified experts can misread x-rays on occasion,” he wrote, “but this record belies the notion that the errors by Drs. Wheeler [and two colleagues] were mere oversight.”
But, to discredit his readings and award benefits to a miner, as Levin did, judges must identify a logical flaw or some other reason not to give his opinion greater weight than those of other doctors. Former judges said they knew certain doctors almost never found black lung, but said they were barred from taking these experiences in other cases into consideration. In four cases reviewed by the Center, judges who have questioned Wheeler have seen their decisions vacated by an appeals board.
Retired judge Edward Terhune Miller, who often saw Wheeler’s opinions in cases before him, said he sometimes was compelled to deny claims even when he had serious doubts about the opinions of coal-company experts from Hopkins and elsewhere. Miners often were unable to provide enough evidence to overcome these opinions, and he wasn’t allowed to take his personal knowledge of doctors’ tendencies into account. “That’s one of the frustrations in the process,” said the former judge. “There’s no doubt about it.”
Wheeler said he is sure miners who don’t have black lung are being wrongfully compensated. “They’re getting payment for a disease that they’re claiming that is some other disease,” the doctor said.
He takes issue with a law passed by Congress in 1969 that was crafted to lessen the burden of sick miners while limiting coal companies’ liabilities. Benefit payments for a miner start at just over $600 a month and max out at about $1,250 monthly for a miner with three or more dependents. Because these caps are low and miners are presumed to be at a particular risk for the disease, the system does not require they prove their cases beyond all doubt. Still, miners must show that they have black lung and that, because of it, they are totally disabled. About 85 percent of claims are denied at the initial level.
“I think if they have [black lung], it should be up to them to prove it,” Wheeler said. To him, this means undergoing a biopsy. If miners don’t submit to the procedure, he said, it suggests they may be afraid the results will show they have something other than black lung.
“I think if they have [black lung], it should be up to them to prove it.”
Dr. Paul Wheeler, radiologist for Johns Hopkins
Biopsies are rarely necessary to diagnose the disease and can put the patient at risk, according to the American Lung Association, the National Institute for Occupational Safety and Health (NIOSH), the Labor Department, a paper published by the American Thoracic Society and prominent doctors interviewed by the Center.
Told his higher standard of proof, which he maintains is ordinary medical practice, is not required by law, Wheeler held firm.
“I don’t care about the law,” he said.

‘Victimized twice’
To people in the southern West Virginia town of Glen Fork, he is “Steve” — longtime miner, father of three, Vietnam veteran. To Dr. Paul Wheeler, from his vantage 400 miles away, he was “Michael S. Day Sr.,” 58, another referral from corporate defense firm Bowles Rice LLP.
Wheeler has never been in a coal mine or met Steve Day. His opinion, though, proved crucial in Day’s case.
In 2004, after more than three decades in jobs that exposed him to high levels of dust, Day’s breathing worsened to the point his doctor urged him to get out of mining. In January 2005, he filed a claim for federal black lung benefits.
The Labor Department pays for a medical examination by a doctor from an approved list. Day unwittingly chose a doctor who commonly testifies for coal companies, yet even this physician diagnosed the most advanced stage of complicated black lung.
Then the opinions from Johns Hopkins began arriving.

A CT scan interpretation by Dr. John Scatarige, who is no longer at the university: Large masses in the lungs, probably tuberculosis, or maybe a fungal disease, or cancer. Black lung unlikely.
Two X-ray readings by radiologist William Scott Jr., with the university since the early 1970s: Large masses in the lungs, probably tuberculosis. Black lung unlikely.
And, most vitally, three X-ray readings and a CT scan interpretation by Wheeler: Large masses in the lungs, probably tuberculosis, histoplasmosis or a similar disease. Black lung unlikely.
Peabody subsidiary Eastern Associated Coal Corp.’s chosen pulmonologist to review the evidence, Dr. Robert Crisalli, originally found black lung but changed his opinion after seeing Wheeler’s interpretations. He adopted most of Wheeler’s views and testified, “The basis for the conclusions primarily centers around the imaging, including the CT scans.”
Day lost.
A spokesman for Peabody spinoff Patriot Coal Corp., which now owns the subsidiary that employed Day, declined to comment, as did a spokesperson for Peabody.
Like many miners, Day relied primarily on the opinion of the doctor who examined him for the Labor Department and the records from his treatment over the years. He was at a distinct disadvantage, squared off against the radiologists at Johns Hopkins.
In determining Day didn’t have black lung, the Johns Hopkins experts relied on the same criteria they have recited in countless cases reviewed by the Center. Put simply, the white spots that show up on film must have a particular shape, appear in a specific area of the lung and follow a specific pattern.
At the Center’s request, a physician not involved in the case, Dr. John E. Parker, reviewed Day’s X-rays and CT scans taken between 2003 and 2012. Parker worked at NIOSH for 15 years, much of the time as director of the X-ray surveillance program and the program to certify qualified readers. He is now chief of pulmonary and critical care medicine at the West Virginia University School of Medicine, and travels the world teaching doctors to read X-rays in seminars, many for NIOSH and the American College of Radiology.
Parker was told only Day’s name, age, number of years mining and the fact that the interpretation of the films was disputed.
His clear-cut conclusion: Complicated black lung. “Based on my findings in reviewing this case, and the classic nature of the medical imaging and history, I am deeply saddened and concerned to hear that any serious dispute is occurring regarding the interpretation of his classically abnormal medical imaging,” Parker wrote. “If other physicians are reaching different conclusions about this case … it gives me serious pause and concern about bias and the lack of scientific independence or credibility of these observers.”
Told later that Day had lost his case, Parker was taken aback.
“It breaks my heart,” he said. “This man has been victimized twice — once by the conditions that allowed him to get this disease and again by a benefits system that failed him.”
Johns Hopkins experts help defeat hundreds of claims
The Center’s review of thousands of cases suggests there are many more men like Day. Since 2000, miners have lost more than 800 cases after at least one doctor found black lung on an X-ray but Wheeler read it as negative. This includes 160 cases in which other doctors saw the complicated form of the disease.
George Hager, for example, worked in the mines for 37 years, and three doctors saw complicated black lung on his X-rays and CT scan. Three Johns Hopkins radiologists, including Wheeler, saw something else — perhaps tuberculosis or histoplasmosis. The judge noted the affiliation of the Johns Hopkins doctors and their “superior qualifications.” Hager lost.
Douglas Hall’s 27 years underground came to an end at the advice of his doctor; he couldn’t walk 100 feet without struggling for breath. Four doctors read his X-rays as complicated black lung, but, again, three Hopkins radiologists, Wheeler among them, graded them as negative, finding tuberculosis or histoplasmosis more likely. Though tests for both diseases came back negative, Hall lost.
Keith Darago initially won twice. Three doctors saw complicated black lung on his X-rays and CT scans, and Administrative Law Judge Linda Chapman rejected attempts by the three Johns Hopkins radiologists to attribute the masses on the films to tuberculosis or a similar disease, particularly given Darago’s negative tuberculosis test and lack of history of any other disease.
But the Benefits Review Board, the highest appeals court in the administrative system, vacated the award of benefits twice and, at the coal company’s lawyers’ request, referred the case to a different judge. This time, the judge found the evidence on film to be a wash. Darago lost.
Some miners or their surviving family members continue to file claims, occasionally winning after their disease worsens or they die. Others simply give up, tired of fighting.
“I think it’s a bad deal,” said Rodney Gibson, another miner whose case followed a similar pattern. All the evidence of complicated black lung he presented wasn’t enough. “They come out with a way of getting around it somehow,” he said.
An X-ray of Steve Day’s chest, taken in 2009, shows two large masses (indicated by arrows). On previous films, Dr. Paul Wheeler said the masses likely were caused by tuberculosis or a fungal infection from bird and bat droppings. A half-dozen doctors have interpreted the masses as complicated black lung. Dr. John E. Parker, who used to run the government’s X-ray surveillance program, said this X-ray shows a classic case of the severe disease. Mouse over the X-rays to magnify the images. Images: Yale Rosen (left), licensed CC BY-SA; courtesy of Steve Day family (right)
Normal X-ray

Steve Day’s X-ray

‘Not using the system properly’
Wheeler flips a switch, and a tall panel hums to life, emanating a white glow in the dark corridor where the Pneumoconiosis Section, as the group of Johns Hopkins radiologists is known, does its work. Papers bearing the letterhead of prominent corporate defense law firms sit at work stations, and stacks of folders in a storage closet have names of firms and coal companies written in Sharpie on their sides.
Wheeler places a series of chest X-rays against the panel and describes what he sees.
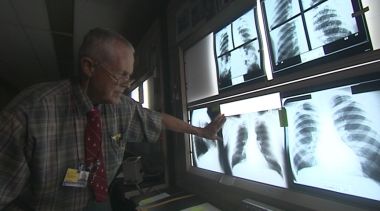
Small white spots obscure much of the lungs on one film, but they don’t have the centralized “birdshot pattern” he’s looking for. “I’d classify it as compatible with coal workers’ pneumoconiosis,” he says. “But I’d also say it certainly could be or more likely is histoplasmosis.”
He moves to films showing large white masses. One doesn’t have small spots surrounding it and is “pretty high [in the lung] — I would call it out of the strike zone,” he says. He again suspects the fungal infection. “If you want to bet against histoplasmosis, you’re going to lose an awful lot,” he says.
These X-rays, however, are not disputed films in a benefits case. They are the standard X-rays that the government says show pneumoconiosis — a family of disease that includes black lung and asbestosis, but not histoplasmosis, tuberculosis and similar illnesses. When reading for pneumoconiosis, government-certified readers are supposed to place the unknown X-ray next to these films; they are classic cases meant to be standards for comparison.
Wheeler questions this and says the classification system has “some quality issues.” He adds, “These are not proven.”
Experts like Wheeler must pass an exam every four years to retain their government certification. If a doctor were to classify these films as negative during that exam, the physician very likely would fail, said David Weissman, director of NIOSH’s Division of Respiratory Disease Studies, which sets the standards for how readings should be performed.
Wheeler, however, has continued to pass the exam for decades, most recently this April.
The form used in the U.S. and many other countries for interpreting X-rays contains boxes to grade what’s on the image and a comments field for further explanation. If spots appear on the X-ray, a reader is supposed to mark their size and shape, and then explain which diseases seem more or less likely.
When he reads X-rays for coal companies, however, Wheeler doesn’t do this. If he sees spots on the film but thinks another disease is more likely than black lung, he marks the film as negative. He typically describes the abnormalities in the comments section, explaining why they don’t meet his criteria for finding black lung. In case after case reviewed by the Center, his comments were almost identical.
Weissman said this approach is simply wrong.
“You’re supposed to grade what’s there,” Weissman said. “You’re not supposed to alter what the grade is based on what you think the underlying cause is. That’s not using the system properly.”
In a statement, university officials said the radiologists “adhere to the clinical standards of diagnosis noted in the guidelines” put forth by the International Labor Organization, upon which NIOSH relies.
Wheeler said he is being more responsible than other doctors by providing multiple possible diagnoses. He often grades the film as negative but says in the comments section that black lung is possible, but unlikely.
The practical effect of Wheeler’s readings: To rule out black lung. Judges may consider the comments he writes, but the key, in comparing Wheeler’s readings with others, is the negative numerical grade he assigns.
In depositions, he sometimes goes further to eliminate black lung as a cause of a miner’s failing health. “He doesn’t have [black lung],” he said in a 2004 case, for example. “[I]n no way is this [black lung],” he said in another.
Weissman said NIOSH often hears that some certified readers interpret X-rays the way Wheeler does and that others over-diagnose diseases. “It’s pretty frustrating sometimes when we hear of people that do well on the exam and then go out in the real world and do other things,” he said. “Absolutely that is a concern.”
The agency’s authority, he said, doesn’t go beyond education, training and administering the exam. People with complaints should contact the state medical board, he said.
No, by the numbers
There is an unmistakable pattern in Wheeler’s readings. The Center identified more than 1,500 cases decided since 2000 in which Wheeler read at least one X-ray; in all, he interpreted more than 3,400 films during this time.
The numbers show his opinions consistently have benefited coal companies:
- Wheeler rated at least one X-ray as positive in less than 4 percent of cases. Subtracting the cases in which he ultimately concluded another disease was more likely, this number drops to about 2 percent.
- In 80 percent of the X-rays he read as positive, Wheeler saw only the earliest stage of the disease. He never once found advanced or complicated black lung. Other readers, looking at the same images, saw these severe forms of the disease on more than 750 films.
- Where other doctors saw black lung, Wheeler saw tuberculosis, histoplasmosis or a similar disease on about 34 percent of X-rays. This number shoots up in cases in which others saw complicated black lung, which is so severe it triggers automatic compensation. In such cases, Wheeler attributed the masses in miners’ lungs to these other diseases on two-thirds of X-rays.
Asked if he stood by this record, Wheeler said, “Absolutely.”
“I have a perfect right to my opinion,” he added. “I found cases that have masses and nodules. … In my opinion, those masses and nodules were due to something more common.”
When his views are questioned, Wheeler often shares anecdotes. He tells the story of performing an autopsy during his residency on a woman thought to have breast cancer; his examination revealed undetected tuberculosis. Other common stories include his father’s severe illness from histoplasmosis and a colleague’s bout with the infection after spending a rainy night in an abandoned chicken coop.
In a case decided in 2010, a doctor disputed Wheeler’s narrow view of black lung, and the miner’s lawyer asked Wheeler during a deposition whether he could cite medical literature to support his views.
“I don’t think I need medical literature,” Wheeler replied.
In a 2009 letter submitted in another case, Wheeler questioned two doctors who read X-rays as positive for black lung and wrote that he and a colleague who had provided opinions in the case “are clinical radiologists at one of the two or three best known hospitals in the world.”
The judge was not impressed. “This self-serving, egotistical diatribe is unwarranted and very unprofessional,” he wrote.
Wheeler took a similar approach in a recent interview, challenging the views of any doctor, judge or organization — including the Labor Department, NIOSH and the International Labor Organization — that contradicted his. He said he’s never been told an interpretation of his was wrong and he’d admit a mistake only if a biopsy or autopsy showed black lung — and was performed by a pathologist with “proper credentials.”
“I know my credentials,” he said. “I’d like to make sure that the people proving me wrong … have … credentials as good as mine.”
Proof in the tissue
In fact, tissue samples from miners’ lungs have proven Wheeler wrong again and again.
The pathologists providing the interpretations were enlisted by the coal company in many cases, and they often came from well-regarded academic medical centers, such as Washington University in St. Louis and Case Western Reserve University, where Wheeler himself was a resident. Some helped write widely accepted standards for diagnosis of black lung with pathology and have been frequent experts for companies defending claims.
Wheeler’s readings were negative even in some cases in which the company conceded the miner had black lung and chose to fight the claim on other grounds.
When clear pathology evidence did exist in cases reviewed by The Center, it tended overwhelmingly to show that the doctors who had found black lung — not Wheeler — were correct.
The American Lung Association, NIOSH, the Labor Department and a paper published by the American Thoracic Society say black lung usually can be diagnosed with an X-ray, knowledge of the miner’s exposure to dust and studies of lung function. Biopsies, which Wheeler insists are “very safe,” are invasive, risky and usually unnecessary, government officials and doctors said.
Still, of the cases in which Wheeler submitted at least one negative reading, miners or their surviving family members submitted evidence from a biopsy or autopsy in more than 280 cases, a Center analysis found. Contrary to Wheeler’s contentions, the pathology did not resolve most cases. In about half, the tissue evidence proved inconclusive or was disputed.
Of the remaining cases, 75 percent revealed undisputed evidence of black lung. In the other cases, the tissue did not show evidence of the disease, but, as the law states, this doesn’t mean the miner didn’t have black lung — only that it wasn’t present on the piece of lung sampled.
In the cases in which pathology showed Wheeler was wrong, other X-ray readers saw black lung 80 percent of the time, and no interpretations outside of Johns Hopkins existed in another 12 percent.
Most times, then, only Wheeler and his Johns Hopkins colleagues failed to see black lung.
Diagnosis after death
Sometimes miners had to die to prove they had black lung.
George Keen worked 38 years in the mines and tried for 22 years to win benefits. At least two physicians interpreted his X-rays and CT scans as showing complicated black lung. Wheeler and his colleague Scott read them as negative — probably tuberculosis, they said. Keen lost.
Three years after the most recent X-rays and CT scans read by Wheeler were taken, Keen died. The company’s chosen pathologist agreed the autopsy revealed complicated black lung.
John Banks, who started loading coal by hand at 17, had multiple claims denied. More than a half-dozen doctors saw black lung; Wheeler suspected cancer. When Banks died, pathologists looking at his lung tissue debated whether the disease had reached the complicated stage, but both sides agreed: He had black lung.
Emily Bolling suffered through much the same experience with her husband, Owen, who spent most of the last six years of his life on oxygen but wasn’t able to win benefits.
“They would keep hiring more doctors and more doctors to read his X-rays, and we had just one,” she said.
Wheeler read a 2002 X-ray as negative. Owen died in 2003, and two pathologists found that the autopsy showed black lung, allowing Emily to win her widow’s claim. “It seems awful, but that’s what it took,” she said recently. “It’s just wrong.”
Illene Barr is trying to win benefits following the 2011 death of her husband, Junior, who worked 33 years doing some of the dustiest jobs in the mines. In his final years, his health progressively worsened. “He loved to do things around the house,” Illene recalled. “He had a garden. But he became so short-winded he couldn’t do any of that. He ended up basically just sitting on the deck.”
He lost claims in 2008 and 2010 after Wheeler read X-rays as negative, saying histoplasmosis was much more likely.
“We just couldn’t believe that it was happening,” Illene said.
Four months after Wheeler’s most recent opinion that Junior likely was suffering from the bird-and-bat-dropping disease, he died. Pathologists for both sides saw black lung on the autopsy. Illene’s benefits case is pending.
The Wheeler standard
Wheeler learned the strict criteria he applies from his mentor, Dr. Russell Morgan, a revered figure at Johns Hopkins. In the early 1970s, Morgan helped NIOSH develop the test to qualify as a “B reader” — a doctor certified to read X-rays for black lung and similar diseases. Wheeler served as one of his test subjects. The radiology department bears Morgan’s name, and he went on to become dean of the medical school.
Morgan testified for companies defending a wave of lawsuits over asbestos-related disease. Wheeler testified before Congress in 1984, arguing that false asbestos claims were rampant and that plaintiffs should prove their cases by undergoing a biopsy. He asserted that similar problems existed in the black lung compensation system.
There is general acknowledgement now that X-ray evidence was misused in some asbestos claims. The black lung benefits system of today, however, is a different universe.
In some asbestos claims, plaintiffs won large verdicts or settlements, and lawyers got rich. For black lung, the payouts are comparatively meager — the maximum monthly payment, for miners with three or more dependents, is about $1,250 — and few lawyers will take cases because the odds of winning and ultimate compensation are low. Settlements are not allowed, and miners have to prove total disability caused by black lung, not just show a minimally positive X-ray.
Wheeler continues to express concerns similar to those he voiced in 1984. “It comes down to ethics,” Wheeler said. “If you think it’s appropriate for somebody with sarcoid to be paid for [black lung] because he has masses and nodules — do you think that’s appropriate? I don’t think so.”
After Morgan’s death, Wheeler took over the “Pneumoconiosis Section.” Asked if he viewed himself as the coal industry’s go-to radiologist, Wheeler said: “Dr. Morgan was the go-to guy. … I’ve replaced him … in the pneumoconiosis section, yes. … I can view myself as the doctor for a number of companies, not just coal companies.”
In depositions and during the recent interview, Wheeler has insisted he is relying on the criteria Morgan taught, praising his predecessor as an innovator and genius. His criteria, however, do not comport with mainstream views on black lung.
“When you take this very strict view, where you put in all these rules, none of which are a hundred percent, what will happen is you’ll wind up excluding people that have the disease,” NIOSH’s Weissman said.
According to medical literature and experts consulted by the Center, black lung does not always fit the narrow appearance Wheeler requires. Shown a text, for example, that says the disease may affect one lung more than the other, Wheeler said: “I don’t know where they get this idea. … It’s not what Dr. Morgan taught me.”
In fact, the statement comes from the standards established in 1979 by the College of American Pathologists. The report was compiled by a group of eminent doctors, including some who have testified regularly for coal companies.
Doctors interviewed by the Center said they had seen many cases of black lung that did not fit Wheeler’s standards. “You’ll see a variety of different presentations,” said Dr. Daniel Henry, the chair of the American College of Radiology’s task force on black lung and similar diseases. “The image can vary.”
In one case decided in 2011, NIOSH got involved at the request of the doctor who examined the miner for the Labor Department. Multiple doctors had diagnosed complicated black lung, but Wheeler had read X-rays as negative. The spots on the X-rays didn’t follow the pattern he wanted to see, he’d said; histoplasmosis was more likely.
Two NIOSH readers, however, saw complicated black lung on the film, and Weissman wrote a letter saying Wheeler’s views “are not consistent with a considerable body of published scientific literature by NIOSH.” The miner won his case.
Assumptions and ‘bias’
A pair of assumptions shapes Wheeler’s views in ways that some judges and government officials have found troubling.
Former miner Gary Stacy’s struggle for benefits lays bare the effects of these beliefs.
When he filed for benefits in 2005, Stacy was only 39 years old, yet three doctors believed his X-rays and CT scans showed complicated black lung. He had worked for almost 20 years underground and had never smoked.
Wheeler, however, read two X-rays as negative. He wrote that Stacy was “quite young” to have complicated black lung, especially since the 1969 law required federal inspectors to police dust levels. Histoplasmosis was much more likely, Wheeler thought.
A judge denied Stacy’s claim in 2008, and it would take years of fighting and a rapid decline in his breathing before he won.
In reaching his conclusions about the cause of the large masses in Stacy’s lungs, Wheeler drew upon beliefs that pervade his opinions: Improved conditions in mines should make complicated black lung rare; whereas, histoplasmosis is endemic in coal mining areas.
In case after case, Wheeler has said complicated black lung was found primarily in “drillers working unprotected during and prior to World War II.”
Wheeler’s contention contradicts a series of published studies by NIOSH researchers showing that the prevalence of black lung actually has increased since the late 1990s and that the complicated form increasingly is affecting younger miners. Wheeler contends these peer-reviewed studies aren’t conclusive because they have not been confirmed by pathology.
Gary Stacy is the kind of miner NIOSH says it now sees more often. Just 47 today, he appears trim and healthy, but a few minutes of conversation reveal a different reality. His sentences are interrupted by hoarse gasps for breath.
Stacy now undergoes pulmonary rehabilitation to prepare for a lung transplant. As his illness worsened, the evidence became overwhelming, and his employer agreed to pay benefits.
The fact that nothing in Stacy’s medical history indicated he’d suffered from histoplasmosis or tuberculosis didn’t prevent Wheeler’s readings from being credited in the 2008 denial. Someone could be exposed, show no symptoms and still develop masses that remain after the infection has fizzled out, Wheeler often has said.
This is theoretically possible, said doctors consulted by the Center, including an expert on histoplasmosis at the Centers for Disease Control and Prevention. But, doctors noted, in cases with masses as large as the ones Wheeler often sees on film, the patient likely would show symptoms and have some record of the disease in his medical history.
NIOSH’s Weissman said the two diseases should rarely be confused on film. “The appearance of [black lung] is different from the typical appearance of … histoplasmosis,” he said. “That shouldn’t be hard, in general, to make that differentiation.”
Wheeler’s main alternative suggestion once was tuberculosis, but he has switched to suggesting histoplasmosis more often. “Well, initially, I thought TB was … causing these things,” he said in an interview. Yet many of those cases, he now believes, “very likely were [histoplasmosis].”
Could he be wrong again? “I could be,” he said. “But I’d like to be proven wrong with biopsies.”
In written opinions, judges have said Wheeler’s assumptions seem to have “affected his objectivity” and “inappropriately colored his readings.” Another wrote in 2011 that Wheeler had a “bias against a finding of complicated [black lung] in ‘young’ individuals.”
In some cases, judges have questioned Wheeler’s demands for biopsy proof and his speculative suggestions of other diseases. “The reasonable inference to be drawn from Dr. Wheeler’s report and testimony is that he does not accept a diagnosis of [black lung] based on x-ray or CT scan alone,” one judge wrote in 2010.
Another judge succinctly summarized Wheeler’s opinion: “I don’t know what this is, but I know it’s not [black lung].”
Scraping to get by, struggling to breathe
Steve Day’s wife, Nyoka, sleeps lightly. Most nights, they re-enact the same scene.

Steve sleeps upright in a recliner; if he lies flat, he starts to suffocate. Nyoka lies in bed in the next room over, listening to his breath and the hiss of the machine pumping oxygen through a tube in his nose. She waits for the sound — a faint gasp.
“I hurry in here, and I bend him over and say, ‘Steve, cough,’ ” she said. “He’ll try and get by without having to cough because it hurts. And I make him cough. I’ll scream at him, ‘Cough!’ ”

What finally comes up is often black. They’ve made it through another night.
This is not the life they envisioned when Steve returned from Vietnam and they eloped. Both of their fathers had worked in the mines, and both had black lung. Before they got married, Steve made Nyoka a promise: He’d never go to work in the mines.
It wasn’t long before he changed his mind, persuaded by his father. “He said that’s the only way you can make good money,” Steve recalled of the job that, in good years, earned him as much as $55,000 or $60,000. He worked just about every job underground. For much of his career, he ran a continuous mining machine, which rips through coal and creates clouds of dust.
“When he came out of the mines, all you could see was his lips, if he licked them,” Nyoka recalled. “He was black except around his eyes.”
After 33 years in the mines, he thought the cause of his breathing problems was obvious. So did his doctor, who is treating him for black lung.
The reports from Johns Hopkins floored Steve and Nyoka. There was nothing in his medical records to suggest he’d ever had tuberculosis or histoplasmosis, let alone a case so severe that it left behind multiple nodules and masses, including one occupying almost a third of one of his lungs.
Steve scowls at the mention of Wheeler’s name. “The more I talk about him the madder I get,” he said. “And the madder I get, my blood pressure shoots up.”
Administrative Law Judge Richard Stansell-Gamm determined, based on the opinions of Wheeler and the pulmonologist who adopted most of Wheeler’s findings, that Day had not proven he had black lung. The judge didn’t come to any conclusions about what caused Day’s severe illness.
He lost his case on May 31, 2011, and, three days later, the Labor Department sent Day a letter demanding $46,433.50. The department had originally awarded Day’s claim in 2005 and started paying benefits from a trust fund because the company’s lawyers had appealed. Now that the initial award was overturned, the department wanted reimbursement for what it paid out during the six years it took for the case to reach a conclusion.
The department eventually waived the so-called “overpayment” after Day submitted documentation showing he had to support, to varying degrees, eight other people with only Social Security and a union pension.
“Each person of age tries to help but overall it isn’t enough to survive on without borrowing,” he wrote the department. “It has been very humiliating to have to do so, when everyone knows that I worked my life away from my children and my wife, in order to end up on full time oxygen for a company who isn’t (decent) enough to acknowledge the damage ‘their’ job done to my body, my life, and my family.”
Day has not given up hope of winning benefits, but, if he files again, he could find himself again having to overcome the opinions of Wheeler and his colleague at Johns Hopkins.
As he almost always does, Wheeler testified in Day’s case that he should undergo a biopsy. Parker, the former NIOSH official who examined Day’s X-rays and CT scans, said he’d advise against a biopsy because the risk of complications for someone with Day’s level of disease is too great.
That leaves just one way, in Wheeler’s opinion, to disprove him. Steve and Nyoka have already discussed it. “I done told her, ‘If something happens to me, have an autopsy done on my lungs,’ ” Steve said.
Since he lost his case, Day’s breathing has declined. He began full-time oxygen a year ago, but decided against a lung transplant. At 67, with his health problems, he likely would not be a good candidate.
Miners have developed a crude measure for how damaged their lungs are based on how upright they need to be to sleep.
“You start out with one pillow,” Nyoka said. “Then you go to two pillows. Then three pillows, and that’s supposed to be your top. Well, he went through that, and he got to where he couldn’t breathe. So he got in the recliner, and he’s just lived in that recliner for …”
“Years,” Steve interjected, staring out the window toward the tree-lined hillside.
“And now the recliner,” Nyoka said. “It’s not enough.”
Editor’s note: Brian Ross and Matthew Mosk work for ABC News. Retired judge Edward Miller’s daughter is employed by the network. The Center contacted him before ABC News joined the reporting for this story.

